IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
VENTILATOR-ASSISTED LIVING
VOLUME 29, NUMBER 3
JUNE 2015

JOANNE KOCOUREK, WORTH, ILLINOIS
Part 1: Our Family Situation/Experience
Psychologists debate what makes a good parent. There is general agreement that good parents love their children unconditionally, make provision for their children’s needs, and provide a home filled with love, security and good times. However, in families caring for children with rare diseases, parents are also grappling with their child’s medical condition, with managed care, insurance benefits, educational issues and the drain on family resources.
According to the National Institutes of Health (NIH), a disease is considered rare if it has a prevalence of fewer than 200,000 affected individuals in the United States. There are roughly 7,000 rare diseases currently identified........MORE
Case study: Tony Tong
Condition: High level spinal cord damamge/trauma
At 22 years old, University of New South Wales Law Student Tony Tong had the world at his feet.
All that changed in 2012 when he received the devastating news that the cause of his underlying lethargy and weakness was a malignant brain tumour, an astrocytoma in the brainstem..........MORE
ADDITIONAL SECTIONS
Networking
Sharing the work of others.
Ventilator Users Speak
Answer questions; learn from others.
Educational Opportunities
Conferences and webinars for health professionals and ventilator users.
Recent Relevant Publications
Summaries, links to selected professional, disability, disease journals and newsletters.
Advocacy
Educate, discuss, take action.
Industry
The business of living with a ventilator.
Supported by:
Ventilator-Assisted Living
Vol. 29, No. 3, June 2015
Editor: Joan L. Headley
Designer: Brian Tiburzi
ISSN 1066-534X
© 2015 Post-Polio Health International.
Permission to reprint must be obtained from Post-Polio Health International (PHI) at info@post-polio.org.
Ventilator users, health professionals, non-profits, company representatives – send comments and updates to info@ventusers.org.
Caring for Children with Rare Diseases: "NORMAL" is What You Make It
JOANNE KOCOUREK, WORTH, ILLINOIS
Part 1: Our Family Situation/Experience
Psychologists debate what makes a good parent. There is general agreement that good parents love their children unconditionally, make provision for their children’s needs, and provide a home filled with love, security and good times. However, in families caring for children with rare diseases, parents are also grappling with their child’s medical condition, with managed care, insurance benefits, educational issues and the drain on family resources.
According to the National Institutes of Health (NIH), a disease is considered rare if it has a prevalence of fewer than 200,000 affected individuals in the United States. There are roughly 7,000 rare diseases currently identified.

(l-r) Annalies, Tom, Joanne, Kristen and (front l-r) Stitch(es), Brooklyn and Skittles
Discovering that your child has, or you yourself have, a rare disorder can come as a great shock. When our youngest daughter was diagnosed with a rare disease I felt a mixture of emotions; sadness, confusion, numbness, anger, guilt, "why me?", isolation, bewilderment and even a sense of bereavement, sometimes sadly literal but very often a sense of grief for the child my husband and I had eagerly awaited. I felt overwhelmed at my lack of knowledge about my child's condition. Even as a nurse by profession, I was confronted by a host of diseases, many that had no name and were extremely difficult to diagnose.
The needs of those parenting children with chronic medical conditions - even those with the same disease process - can vary tremendously. I’d like to take you on a journey. This particular journey is very personal. It is the path less trodden that our family ventured upon when seeking answers to the question, “What is wrong with my baby?” which soon became, “What is wrong with our daughters?”
The Journey
Tom and I had what some might call an ideal situation. We were happily married, lived in a modest home in the suburbs of Chicago and were the proud adoptive parents of two presumably healthy children, Joshua and Annalies. Unexpectedly, our adoption agency called to inquire if we would be willing to add a third child to our family. The answer was a resounding yes. This query came because Annalies’ birthmother had recently met with the adoption agency, informed them that she was expecting another baby and she desired that her biological children be raised as siblings, if at all possible.
Kristen was born on November 28, 1989 with great anticipation. At the time of her birth, it was obvious that she had some unexpected health issues. Kristen was extremely cyanotic and an echocardiogram revealed a mix of correctable congenital heart defects. No problem. Kristen would receive the best pediatric cardiac care that was available.
Nine weeks after she was born, Kristen was found grey in color, pulseless and not breathing while asleep. Cardiopulmonary resuscitation was successfully initiated. She was admitted to a local hospital where no common abnormalities could be found. The only concern was an abnormal pneumogram which demonstrated hundreds of apneic episodes and she was discharged to home with an apnea monitor.
The apnea monitor bellowed its resounding alarm with great frequency. In an attempt to determine the cause for recurrent apneic and bradycardic events, our family physician admitted her into the hospital for additional testing, which again showed no explanation for the problem. For the next two years, our baby was slow to grow, had very little energy for play and had recurrent apneic and bradycardia events.
At age two Kristen was admitted for extensive clinical monitoring during which a more formal sleep study was performed. It revealed that she had apnea episodes with hypoxia, hypercarbia and obstruction. A computed tomography scan was performed which revealed that Kristen’s trachea was being compressed by an aberrant subclavian artery. Surgery was performed hoping that in relieving the tracheal compression, the apnea, bradycardia and cyanotic episodes would resolve.
At the time of this cardiac surgery, it was determined that the congenital heart defects had almost all completely self-resolved. Kristen seemed to improve with more energy, less apnea, minimal bradycardia and less cyanosis for four to six months.
Then with the onset of a typical otitis media, it seemed that all of the clinical improvement was immediately gone. By this time, I’d completed an extensive Medline Search and read countless articles relating to disorders of respiratory control in children. The only disease that seemed to fit her clinical picture was something called Congenital Central Hypoventilation Syndrome.
Kristen was once again admitted to the hospital for an extensive evaluation, and this time, in July of 1992, the physicians confirmed the diagnosis that we had been searching for, Congenital Central Hypoventilation Syndrome or CCHS or Ondine’s Curse.
This was based on their findings of bradycardia, apnea, high retained CO2 levels in her lungs from inefficient respiratory function awake and asleep, no heart rate variability, no ventilatory responses to changes in oxygen or CO2. All of the additional clinical studies that were done seeking other disease states or process that could cause these findings came back negative. It should be noted that not all children exhibit the same traits.
In layman's terms, CCHS means the neurological absence of the appropriate trigger mechanisms to provide adequate breathing over an extended period of time. CCHS was discovered in the late '70s with the advent of pediatric respirators that provided the mechanism to recognize and treat the symptoms. With increasing knowledge of CCHS and different treatments modalities, CCHS is now considered a treatable disorder, which will be included in Part 2 in the next issue of Ventilator-Assisted Living.
Our Journey Continues: Another Affected Child
The picture of perfect health: Annalies! She was our healthy child. Throughout early childhood Annalies had minimal health issues - mild hypotonia (though to be secondary to prematurity), hyperactivity and a rare migraine headache. That picture of healthiness evaporated for her with the onset of puberty.
It seemed like overnight, the hyperactivity was replaced by excessive sleepiness. New clinical signs and symptoms emerged almost daily. Our family doctor diagnosed the following over a two month period of time: ventricular tachycardia, supraventicular tachycardia, neurocardiogenic syncope, hypoxia, stroke-type events, mixed seizure activity, liver function abnormalities, migraine headaches, gastrointestinal dysmotility, asthma, apnea secondary to airway obstruction, cyclic vomiting and immune function abnormalities.
Her primary respiratory issue was Obstructive Sleep Apnea Syndrome. As the muscles of her airway become weaker she has experienced more apnea, hypoxic and hypercarbic insult. Neither our family physician nor any of the local physicians consulted could explain what was happening. They all agreed that it was likely Annalies’ medical issues where in some way related to the myriad of medical problems Kristen had, but no one could come up with an explanation.
Once again, a subspecialist that thought outside of the box agreed that a relationship was probable and the search for a global diagnosis was initiated. That physician and I conducted a massive Medline and internet based search for an explanation and the likely culprit was Mitochondrial Cytopathy (Mitochondrial disease is a rare, chronic, genetic disorder that occurs when the mitochondria of the cell fail to produce enough energy for cell or organ function. There are many forms of mitochondrial disease with clinical presentations that vary widely from individual to individual.).
In an attempt to obtain a formal diagnosis, Annalies and Kristen were referred to several physicians specializing in diagnosis and management of Mitochondrial Disease, and after obtaining numerous laboratory studies and fresh muscle biopsies we were presented with a very bewildering diagnosis: Mitochondrial Cytopathy.
Fast forward to 2015, both daughters now have clinical and genetic confirmation of two rare or unique diseases: Congenital Central Hypoventilation Syndrome and Mitochondrial Cytopathy. A recent clinic visit with a nationally recognized dysautonomia specialist yielded this comment, “Your daughters have the distinction of having two diseases which together create some of the worst dysautonomia I have ever seen and require the highest level of homecare support available to maintain the ability to live and have a great quality of life.”
Tips from the Trenches
I know how much it can help to talk to people who understand. Our daughters, now young women, often talk of the tremendous difference it makes to locate and communicate with others who “get it.”
-
Have a good support system in place.
-
Ask for help and thoroughly investigate community resources.
-
Never take NO for an answer.
-
Nothing is impossible.
-
Expect some negative feelings and move on.
-
The joy the child(ren) brings far outweighs the downside of managing the disability.
-
Learn everything you can about the child’s/individual’s condition and unique needs.
-
Learn what the standards of care and treatment are for the particular condition.
-
Evaluate health plans before you enroll in detail to ensure that they will meet your child’s needs.
-
Physicians are your most influential allies, particularly when the going gets rough.
-
Determine if there is a medical group in your community that can specifically treat/manage children with their particular disease state.
-
Document everything.
-
Challenge decisions and be persistent.
Part 2: The Solutions/Resolutions and Ventilator-Assisted Living will be in the next issue.
I could sum it up in one word: Freedom
Case study: Tony Tong
Condition: High level spinal cord damamge/trauma
At 22 years old, University of New South Wales Law Student Tony Tong had the world at his feet.
All that changed in 2012 when he received the devastating news that the cause of his underlying lethargy and weakness was a malignant brain tumour, an astrocytoma in the brainstem.
In the months after his initial diagnosis, Tony was admitted into the Prince of Wales Hospital in Sydney and began radiotherapy, but that provided little improvement, so surgery was the last remaining option.
“My spinal cord was like a piece of string – all the rest was occupied by the tumour,” Tony remembers.

Caught between either having high-risk surgery or facing certain death, there was little choice.
So in May 2103, Tony underwent surgery by world-renowned neurosurgeon, Dr. Charlie Teo, to remove the astrocytoma from one of the most inaccessible parts of his brain.
The risks were great; to survive was a major achievement. Preserving Tony’s life came with the uncompromising cost of high-level quadriplegia.
Close to complete paralysis, his recovery began with three months in the Intensive Care Unit (ICU) on mechanical life support. There, he still found a way to communicate, although his friends and carers had to learn to lip-read.
“Not being able to vocalize was so incredibly frustrating,” Tony says.
The severity of his quadriplegia required full-time ventilation. Over the course of his stay he switched form the ICU’s heavy ventilators to ResMed’s more compact Elisée™ 150.
Once stabilized, Tony was transferred to the Spinal Rehabilitation Unit where he underwent intensive physiotherapy, and occupational and speech therapy sessions to regain basic skills of life, as well as his independence.
“I kept visualizing getting out of hospital, finishing university and getting my career on track,” he says.
“I wanted to pick up where the happiness had stopped.”

Set up with a computer, which operated through voice recognition and a QuadJoy hands free mouth mouse, Tony was optimistic. He wanted to attend lectures, catch public transport and remain social like everyone else.
In March 2014, Tony was introduced to Astral™. Fitted to his wheelchair, the smaller portable ventilator with long battery life and a range of therapy settings, gave doctors and nurses more options to better meet Tony’s needs, and provided him with mobility.
“Just being able to go out without the constant pressure that if I don’t go back in a few hours I’ll die, has made a huge difference,“ Tony says.
“Simple pleasures such as visiting the shops or going out for dinner are now so much more possible.”
After 16 months of hospitalization, Tony was discharged in September 2014. He now lives at home with his fiancée, Ashanti, and his cat, Leo.
In his most important decision and every related one afterwards, Tony chose life. He is now contemplating when he will graduate with his law degree, what jobs to apply for and where to have his wedding.
Though he remains on 24-hour ventilation and needs a carer at all times, the use of modern ventilation devices makes it less difficult being a quadriplegic and retaining a quality of life – just as Astral did for Tony.
“I could sum it up in one word,” he says, “Freedom.”
PHI/IVUN Research Fund
International Ventilator Users Network reminds researchers about its “Request for Proposals” for research into neuromuscular respiratory conditions.
Deadline is October 1, 2015 (to be awarded in 2016).
Questions? Call 314-534-0475 or email info@ventusers.org.
Networking
CCHS Family Network adds Foundation
Mary Vanderlaan, Executive Director of the CCHS Family Network, reports that the twenty-six year old organization recently created The CCHS Foundation. The aim of the Foundation is to raise money with the purpose of expanding CCHS research (70% commitment), continue educational outreach programs (20% commitment), and assist patients and families living with the condition (10% commitment). It is overseen by a board of directors and regional coordinators.
Melinda Riccitelli and Rebecca Martine serve as Co-Chairs of the Foundation. “This is a very exciting time for our CCHS community,” they said in a statement. “With an approximate1,200 patients worldwide, it has taken many years to gain the necessary momentum to start and ensure a successful fundraising campaign. Researchers believe that better treatments are on the horizon, which has inspired us to launch the Foundation in hopes of accelerating this goal.”
The Foundation has developed a widescale strategic plan designed to raise CCHS awareness while appealing to both private and corporate donors. Grassroots events, marketing through social media, and collaboration on international fundraising activities are underway. You can follow the Foundation at www.facebook.com/TheCCHSFoundation.
Additionally, The CCHS Family Network established a Research Advisory Board (RAB) in 2014 led by Dr. Eddy Yang, medical researcher and CCHS parent, along with a team of US and international CCHS experts. The RAB will be responsible for reviewing applications and awarding grant funds.
Vanderlaan adds, “We are at the end of our first year of a closed, dedicated Facebook discussion group for our families where we confirm each participant family's diagnosis, thereby also creating a so called clean pool of CCHS families/patients.” The discussion page has brought together families from around the world and provided an easy and accessible way to share stories, tips and desires to change the world for CCHS patients.
Congenital Central Hypoventilation Syndrome is a multisystem disorder of the central nervous system where, most dramatically, the automatic control of breathing is absent or impaired. A CCHS patient’s respiratory response to low blood oxygen saturation (hypoxia) or to CO2 retention (hypercapnia) is sluggish during wake hours and absent to varying degrees during sleep, serious illness, and/or stress. Studies suggest that up to 17% of CCHS children may require 24-hour ventilation support. Complications associated with CCHS include seizures, Hirschprung’s disease, cancer, and developmental delays. There is currently no medication and patients must rely on mechanical ventilation via tracheostomy, BiPap or phrenic nerve pacers.
The dedicated work of the CCHS FAMILY NETWORK, over the years, has helped improve the lives of children with CCHS, who today with appropriate treatment are now in their 30s and 40s. CCHS young adults are in college, in the workplace, and some are having their own families. With the establishment of the CCHS Foundation, this rare orphan disease could see new developments that were once considered a “dream.”
Global Tracheostomy Collaborative
Initiated in July 2012, The Global Tracheostomy Collaborative (GTC) was created because, quoting Dr. David W. Robinson in an article in Talk Muir, “trach patients are at high risk for serious or catastrophic adverse events and that, tragically, many of these events can be prevented.”
The Collaborative hosted kickoff events in 2014 with more scheduled for 2016. Thirty hospitals have joined GTC, which recommends that hospitals consider five key drivers: multidisciplinary teams, standardization of care, meticulous education of staff, family involvement and outcome tracking. The GTC is coordinating a database for its members to use to track each individual.
Visit www.globaltrach.org to join as an individual healthcare provider (free), a patient/family member (free) and to learn how to join as a hospital.
Click here to read more in Talk Muir on page 6-9.
Ventilator Users Speak
Comment about results of IVUN survey presented at JIVD/ERCA
“I would like to suggest that the concern about end-of life issues is low on the list because many ventilator users have already addressed it.
“I am mostly ambulatory, require a ventilator which I use noninvasively about 14 hours a day, and currently have pulmonary hypertension from underventilation. I am in the process of being fitted for a power chair that can carry the ventilator.
“In the past six months, I have had 12 doctor's appointments, two ER visits, two brief hospital stays and two trips to my lawyer to update my will and power of attorney for healthcare (POA).
“At seven visits, the first questions asked led to an extensive discussion about end-of-life issues. At four visits, I was told that I MUST decide now whether I want a tracheostomy or not, in case I am brought in with pneumonia or an accident and must be intubated. I was told that I MUST decide now and tell my adult son now exactly at what level of severity to cease resuscitation efforts. Both decisions must be put in writing in my healthcare power of attorney for healthcare.
“These are routine questions in the US. So, those who have not thought about end-of-life issues must not have been in the hospital lately. My impression was and is that most of the medical personnel I have encountered feel that anyone on a ventilator must be at death's door. (I don't think I look deathly ill.) They don't see this as a chronic situation, but rather as an indication of imminent demise.”
Bonnie Jo Grieve
Educational Opportunities
CHEST Course
Mechanical Ventilation: Advanced Critical Care Management, July 30 - August 1, 2015, Innovation, Simulation, and Training Center, ACCP, Glenview, Illinois, USA.
European Respiratory Society Congress in September
September 26-30 are the dates for the European Respiratory Society International Congress 2015 in Amsterdam. Click here for access to the Programme, which will only be available in digital format. No print materials will be distributed.
VENTure eVent in New York
October 19, 2015 is the date for 2nd Annual VENTure eVent - Information Technology and Communication Access for Vent Users – at the CEWIT2015 Conference at the Melville Marriott Long Island, New York. For more information, contact Pam Block (Pamela.Block@stonybrook.edu) at VENTure Think Tank at Stoney Brook.
FOCUS Fall 2015
Focus Fall 2015 will be held September 28 & 29, 2015 at The Desmond Hotel & Convention Center in Albany, New York and at Bally's Hotel in Las Vegas on October 21 & 22, 2015.
CHEST 2015 in Montréal
October 24-28, 2015 are the dates for CHEST 2015 in Montréal, Canada. FYI: Problem-Based Learning Sessions include “Cough Guidelines” on Tuesday, October 27 and “Home Mechanical Ventilation Guidelines”on Wednesday, October 2. The CHEST Simulation Center features “Initiating Home-Based Ventilation” on Tuesday, October 27, 9:00 am to 10:00 am.
AARC Congress 2015 in Tampa
American Association for Respiratory Care (AARC) Congress 2015, The 61st International Respiratory Convention & Exhibition, will meet in Tampa, Florida, November 7 - 10, 2015.
Recent Relevant Publications
From American Thoracic Society
“Hypoventilation and nocturnal desaturations in neuromuscular disease are due to the combined effects of reduced lung volumes during supine sleep and sleep-disordered breathing subsuming phasic REM-related pseudocentral events, desaturations, hypoventilation, obstructive and central sleep events” is part of the conclusion in "Sleep-disordered Breathing in Neuromuscular Disease" by Loutfi S. Aboussouan in the American Journal of Respiratory and Critical Care Medicine, Vol. 191, No. 9 (2015), pp. 979-989.
“Families need to be given a voice regarding what treatments are consistent with the patient’s values and preferences, and physicians’ professional integrity also needs to be respected, meaning that they should not be compelled to administer treatments that violate good medical practice,” is a quote from one of the co-chairs of the committee that helped develop New Guidelines to Resolve Conflicts in Treating Critically Ill Patients. The guidelines were published in the June 1, 2015 issue of the American Journal of Respiratory and Critical Care Medicine.
From the American College of Chest Physicians
“Similar to a train stopping to refuel and exchange passengers, a palliative care consult is a chance for a patient, family, and medical provider to get off the train and do two important things.”
"Palliative care as a train station" in CHEST™ Physician, Vol. 10, No. 4, April 2015, pg. 44, by Dr. David Kregenow.
About SERVE-HF
SERVE-HF is a multinational, multicenter, randomized controlled Phase IV study that was designed to assess whether treatment of moderate to severe predominant central sleep apnea with ASV therapy in addition to optimized medical care could reduce mortality and morbidity in patients with symptomatic chronic heart failure. ResMed reported that ”preliminary analysis of the data identified a statistically significant 2.5 percent absolute increased risk of cardiovascular mortality for those patients in the trial who received ASV therapy per year compared to those in the control group.”
For details:
-
Healthcare providers and patients who have questions or would like more information are encouraged to call 1-800-478-9010 and visit www.SERVE-HFFAQs.com.
For adolescents
New Transition Guide: The Oregon Council on Developmental Disabilities has produced a new transition guide, Planning My Way to Work: A transition guide for students with disabilities leaving high school. The guide contains information for young adults and family members about transitioning to adulthood, and covers special education, transition services, Vocational Rehabilitation, Developmental Disability services, Social Security, housing, health care and more. The guide will soon be printed in Spanish, Russian and Vietnamese. You can order FREE print copies online.
Voicing My CHOICES™: A Planning Guide for Adolescents and Young Adults (© 2012) is a 15-page booklet designed to provide a way to express thoughts about how younger people with serious illness would want to be comforted, supported, treated and remembered. The booklet was developed by researchers at the Pediatric Oncology Branch, National Cancer Institute and the National Institutes of Mental Health at the National Institutes of Health.
For 2015-2016 northern hemisphere influenza season
The recommended composition of influenza virus vaccines is an A/California/7/2009 (H1N1)pdm09-like virus; an A/Switzerland/9715293/2013 (H3N2)-like virus; a B/Phuket/3073/2013-like virus. It is recommended that quadrivalent vaccines containing two influenza B viruses contain the above three viruses and a B/Brisbane/60/2008-like virus.
The recommendation is the same for use in the 2015 southern hemisphere winter. A/South Australia/55/2014, A/Norway/466/2014 and A/Stockholm/6/2014 are A/Switzerland/9715293/2013-like viruses.
Advocacy
NAMDRC Report: Physician and patient groups weigh in on outdated CMS policy
International Ventilator Users Network is one of the patient groups following the discussions between the National Association for Medical Direction of Respiratory Care (NAMDRC) and the Centers for Medicare & Medicaid Services (CMS). NAMDRC is a national organization of physicians whose mission is to educate its members and address regulatory, legislative and payment issues that relate to the delivery of healthcare to patients with respiratory disorders. IVUN will write letters, respond to inquiries and involve its Membership as needed to help assure access to appropriate equipment.
Industry
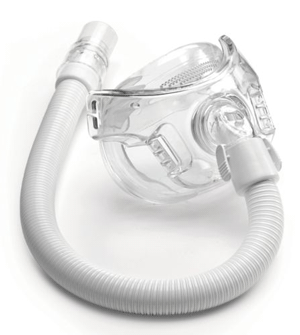
Amara View
Full face mask from Philips Respironics
The Amara View has an under-the-nose design that won’t cause red marks on the bridge of the nose. It is also the small, lightweight and has a wide field of vision. It’s easy to wear glasses, read, watch TV, and use a computer or tablet before falling asleep. It is a vented mask.

Lumis Series Launched in Europe by ResMed
In late April 2015, ResMed announced its new series of noninvasive ventilation devices joining the Stellar and Astral lines.
The series of bilevel positive airway pressure devices comprises the following.
Lumis™ 100 VPAP S features include Vsync, TiControl™ and Trigger and cycle technology, heated humidification capabilities and automatic optimal humidification and ramp.
Lumis™ 100 VPAP ST has, in addition to the above, Intelligent Backup Rate (iBR).
Lumis™ 150 VPAP ST additionally features iVAPS (intelligent Volume-Assured Pressure Support) mode and optional AutoEPAP that auto-adjusts expiratory pressure.

Global Facial Interfaces Market 2015-2019
March 2015, Infiniti Research Limited (103 pages)
Facial interface devices help in treatment using noninvasive ventilation and CPAP therapy. Facial interface devices include all types of masks (nasal pillow masks, nasal masks, oral masks, and full-face masks) and humidifiers that provide airflow into the nose or mouth from breathing machines.
TechNavio's analysts forecast the Global Facial Interfaces market to grow at a CAGR of 6.80 percent over the period 2014-2019. For more details and to purchase.
Class II Recall
ResMed voluntarily reported to the Food & Drug Administration a Class II recall of Astral 100 (Model No. 27001) & Astral 150 (Model No. 27003) ventilator.
The Astral device allows clinicians to disable all alarms including those that detect circuit disconnection. Inappropriate disabling of alarms in ventilator dependent patients can lead to hazards of insufficient ventilation and insufficient expiratory pressure which can result in major severity harm.





