IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
Home Mechanical Ventilation: The Basics
CONTENTS
What is ventilation?
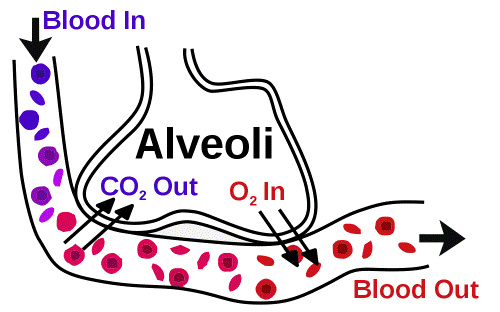
Ventilation is the process by which the exchange of oxygen (O2) and carbon dioxide (CO2) occurs in the alveoli in the lungs. The alveoli are small air sacs at the end of the bronchial tree in the lungs, and it is through the walls of these air sacs that O2 diffuses into the blood and CO2 diffuses out of the blood. Ventilation is a constant process of maintaining the proper balance between the two.
What is mechanical ventilation (MV), also known as assisted ventilation?
Breathing can be assisted mechanically for people who have spontaneous but weak breathing or for people who cannot breathe on their own. Mechanical ventilation (MV), or assisted ventilation, can be used on a short-term or long-term basis, depending on the individual's medical needs.
Short-term use of MV generally occurs in a hospital ICU, e.g., during an acute illness or during and after an operation, until an individual can breathe unassisted. In the ICU, MV can be delivered noninvasively through a face or nasal mask, but is usually delivered by an endotracheal tube placed in the mouth and down the throat (intubation).
In some cases, short-term use of MV in the hospital turns into longer-term use. Generally, if an individual has been intubated for an extended period, such as two weeks, a tracheotomy is performed. This is a surgical procedure that creates an opening in the neck to the windpipe. A plastic or metal tracheostomy tube is placed into the windpipe through this opening. The individual relies on air delivered by a machine through the tracheostomy tube rather than through a tube inserted into the nose or mouth and into the windpipe. When the person becomes medically stable, but still needs to use tracheostomy ventilation, he or she is usually discharged to a long-term acute care hospital (LTACH), a skilled nursing facility or to home care if feasible. Eventually, the individual may be able to breathe unassisted or to be converted to noninvasive ventilation.
Long-term MV may be necessary for extended periods or for life. It may be indicated for some people with stable/chronic conditions such as neuromuscular disease, obstructive lung disease or other conditions that limit the use of the breathing muscles and/or involve the airways.
What are the benefits of using MV?
There are several interrelated benefits that include:
-
maintaining and/or improving the oxygen/carbon dioxide levels in the blood
-
resting the respiratory muscles;
-
decreasing the work of breathing;
-
inflating the lungs more fully;
-
improving cough by stacking breaths;
-
improving sleep quality and breathing during sleep;
-
preventing/avoiding hospitalization for respiratory complications;
-
improving quality of life, and;
-
improving survival.
Who uses long-term MV?
Infants, children and adults who have neuromuscular and/or musculoskeletal diseases and conditions that affect the respiratory muscles, spine and ribs may have reduced lung capacity and/or stiff chests. Their lungs are healthy but they need MV to help augment or take over the work of the respiratory muscles, primarily the diaphragm, during inspiration (breathing in). Some individuals may be able to breathe on their own for most of the day and need to use MV only during the night; others may require 24-hour MV. The diseases and conditions include but are not limited to post-polio; amyotrophic lateral sclerosis (ALS), also known as Lou Gehrig's disease; muscular dystrophy; spinal muscular atrophy (SMA) and scoliosis/kyphoscoliosis.


People who have sustained a high spinal cord injury often need MV if the spinal cord has been injured at or about the fourth cervical vertebra (C4) or higher, and the respiratory muscles are paralyzed. After rehabilitation and special breathing exercises, some individuals are able to breathe on their own for short periods, but, generally, they must use a ventilator for the rest of their lives.
Some people with high spinal cord injuries choose diaphragmatic or phrenic pacing to assist their breathing. This involves an operation to implant electrodes on the phrenic nerves connected to wire leads implanted subcutaneously (under the skin). An external transmitter activates the leads to deliver stimulating pulses to the phrenic nerves, causing the diaphragm to contract. Thus, no ventilator is needed, although many keep the tracheostomy open for suctioning.
Adults with sleep-disordered breathing syndromes such as obesity hypoventilation (underventilation) or infants and children with congenital central hypoventilation syndrome (CCHS) need to use MV only during the night. Children with CCHS may also be good candidates for diaphragmatic pacing.
There are some people who have severe exacerbations of chronic obstructive pulmonary disease (COPD), such as emphysema or chronic bronchitis, or severe cardiopulmonary conditions such as congestive heart failure or cor pulmonale, whose breathing is helped by MV.
Some individuals who have had tuberculosis can also benefit from using MV.
What is a ventilator?
A ventilator is the equipment used to mechanically assist breathing by delivering air to the lungs. Many people may be familiar with ventilators in the hospital setting, such as the ICU, where large complex acute care ventilators are used. The ventilators used in the home are small, lightweight and portable; they can be mounted on wheelchairs or carts or put on a bedside stand. Most of these operate on household electric current. Many have internal batteries, can be operated with external batteries, and newer models features “hot swappable” batteries, extending the time a ventilator user can be away home. It is advisable to have a backup battery or even a generator readily available in case of power outages or emergencies.
How does MV work?
The diaphragm is the primary muscle for inspiration, along with the intercostal muscles between the ribs. Other muscles of the chest, neck and shoulders play smaller roles. When these breathing muscles are weakened or paralyzed, breathing becomes difficult or impossible. A mechanical ventilator can take over the act of breathing completely or make breathing easier by assisting weakened respiratory muscles.
The muscles of the abdomen are important for breathing out (expiration) and for an effective cough. Weak expiratory muscles result in impaired cough and inability to clear secretions that can lead to respiratory infections and pneumonias. In certain neuromuscular diseases, the bulbar muscles – those responsible for swallowing, speech and coughing – can become progressively impaired. Cough can be assisted with the use of manual and/or mechanical methods. There are several cough assists device available, e.g., Comfort Cough™ (Seoil Pacific Group); CoughAssist E70, CoughAssist T70 (Philips Respironics); Mini Pegaso A-Cough, Mini Pegaso A-Cough Perc, Pegaso Cough, Pegaso A-Cough Perc (Dima Italia S.r.l.); Nippy Clearway (B & D Electromedical); Pulsar (Siare Engineering International Group S.r.l.); The Vital Cough™ System (Hill-Rom).
How did mechanical ventilation develop?
The iron lung or "tank" was the first effective form of mechanical ventilation and one of the earliest iron lungs, often used to resuscitate drowning victims, dates from 1838. A century later, in the 1930s, improvements in the iron lung made widespread use of mechanical ventilation possible. Iron lungs are an example of negative pressure ventilators. Other forms of negative pressure ventilation include the chest shell or cuirass, Nu-Mo suit and Pulmo-wrap.
Positive pressure ventilators developed as a more effective breathing option than the larger, bulkier negative pressure devices. Since the 1980s, computer technology has enabled manufacturers to produce even smaller, lightweight ventilators that are easier to transport and operate, and are better suited for people living at home.

What is negative pressure ventilation?
When the pressure around the chest is negative – lower than atmospheric pressure – the chest expands to allow air to enter the nose and mouth. Iron lungs enclose the whole body, except for the head, and create pressure changes between the chest and the encasing shell of the unit. Other forms of negative pressure ventilation, also known as body ventilators, include the chest shell or cuirass, Nu-Mo suit and Pulmo-wrap. The Porta-Lung™ is a small and more mobile version of the iron lung. Today, some people still use an iron lung, chest shell or Porta-Lung™.
All negative pressure ventilation systems provide MV noninvasively to the body – no surgical operation, such as a tracheotomy, is necessary.
What is positive pressure ventilation?
Positive pressure – higher than atmospheric pressure – pushes air into the lungs. It can be administered either noninvasively via a wide variety of nasal, facial and oral masks, nasal pillows (small cushions that fit into the nostrils), and mouthpieces – with tubing attaching to the ventilator or invasively via tracheostomy.
Positive pressure ventilators were developed as a more effective breathing option instead of the larger, bulkier negative pressure devices.
Examples of equipment that deliver positive pressure ventilation are bilevel positive airway pressure ventilators, pressure support ventilators, multi-mode or combination ventilators and volume-cycled ventilators. See IVUN’s Home Ventilator Guide.
The high flow of air from positive pressure may cause dryness in the nasal passages and upper airway, and humidifiers may help relieve symptoms of nasal stuffiness, dry mouth and thick nasal secretions.
An integrated humidifier is a feature of some of the ventilators.
What is noninvasive positive pressure MV?
In noninvasive positive pressure MV, tubing connects the ventilator to the person via an interface. Interfaces include a wide range of nasal, oral or facial masks, nasal pillows (small cushions that fit into the nostrils), and mouthpieces, lipseals or other oral appliances. The nasal and facial masks can be custom-made.
The advantages of noninvasive MV: avoids the need to create an opening in the neck (tracheotomy) that may become a site for infection and irritation, permits normal speech and swallowing (if unaffected by the neuromuscular disease), preserves sense of taste and smell, and reduces need for attendant/personal assistance, family caregivers or nursing care related to MV.
Disadvantages include having the mouth and/or nose covered by the interface, possible upper airway obstruction, inability/claustrophobia in tolerating the mask, and safety issues if 24-hour MV is needed. Noninvasive MV may not be successful, or no longer work, when secretions are heavy and when there is progressive impairment of the muscles responsible for swallowing, speech and coughing, i.e., the bulbar muscles.
An effective cough to remove secretions is vital to the success of noninvasive MV. Cough can be assisted with the use of manual and/or mechanical methods. There are several cough assists device available, e.g., Comfort Cough™ (Seoil Pacific Group); CoughAssist E70, CoughAssist T70 (Philips Respironics); Mini Pegaso A-Cough, Mini Pegaso A-Cough Perc, Pegaso Cough, Pegaso A-Cough Perc (Dima Italia S.r.l.); Nippy Clearway (B & D Electromedical); Pulsar (Siare Engineering International Group S.r.l.); The Vital Cough™ System (Hill-Rom).
Noninvasive positive pressure ventilation is an option for short-term as well as long-term MV.

What is invasive positive pressure MV?
Invasive ventilation is via an endotracheal tube or a tracheotomy (a surgical opening in the windpipe to create an airway through which a tracheostomy tube is placed and connected by tubing to a positive pressure ventilator). Some individuals, such as those with ALS or muscular dystrophy, are unable to use noninvasive MV due to bulbar muscle impairment and/or may not find it as effective as invasive ventilation, particularly if 24-hour ventilation is needed. There are several types of tracheostomy tubes available.
The advantages of tracheostomy positive pressure ventilation include direct access to the upper airway, avoidance of upper airway obstruction, a face free of a nasal or facial mask, and a more secure and safer system when 16- to 24-hour support is needed.
Disadvantages include potential infection, irritation around the tracheostomy, increased secretions upon initiation, increased caregiving due to removal of secretions by suctioning or a mechanical cough device, and more expensive equipment and related supplies. Special attention is needed for speech, such as the use of a speaking valve.

What is sleep-disordered breathing?
People with weak respiratory muscles often experience breathing abnormalities during sleep as the first indication of a problem. Signs include frequent arousals and fragmented sleep, and a reduction in the quality and efficiency of sleep. Underventilation typically occurs during REM sleep, leading to decreases in the level of oxygen saturation and increases in the carbon dioxide in the blood.
Apneas and hypopneas also occur. Apneas are defined as brief episodes when air stops moving in and out of the lungs during sleep for at least ten seconds; hypopneas are episodes when air movement is present but reduced. Some apnea episodes are considered normal; up to five per hour, but an increase in apnea episodes to more than ten per hour indicates the need for evaluation and treatment.
Obstructive sleep apnea (OSA), which is common in the general population, occurs when tissues in the throat collapse, intermittently blocking airflow during sleep. Central sleep apnea occurs when the brain fails to send appropriate signals to the body to initiate breathing, and there is neither airflow nor chest movement. Mixed apnea is a combination of central and obstructive factors occurring in the same episode of sleep apnea.
When sleep apnea is suspected, a sleep study in a sleep laboratory or through home sleep studies can confirm the diagnosis. In people with sleep apnea, the standard treatment is CPAP.
Individuals with respiratory muscle weakness who are experiencing nocturnal breathing problems should be evaluated by a pulmonologist who is experienced in neuromuscular disease to determine whether the cause of the problems is underventilation or sleep apnea or both. Underventilation is optimally managed with MV.
What is CPAP?
CPAP (continuous positive airway pressure) units provide a continuous flow of air under the same level of pressure during inhalation and exhalation to help keep the airway open. CPAP is the standard treatment for obstructive sleep apnea; however, it does not assist with breathing and is not considered ventilation. New auto-titrating CPAP units deliver varying levels of pressures based on the detection of sleep-disordered breathing events and can change pressure on a breath-by-breath basis.
What is a bilevel positive airway pressure ventilator?
Bilevel ventilators were developed by modifying CPAP to also provide inspiratory positive airway pressure (IPAP) to assist inspiration (breathing in). IPAP and expiratory positive airway pressure (EPAP) settings are adjusted separately. People with neuromuscular disease and weak diaphragmatic muscles often may have difficulty breathing in and need IPAP set higher than EPAP, e.g., an IPAP of 14 and an EPAP of 3. The difference between IPAP and EPAP is called the span, and in these cases should be at least 10.
Bilevel units are made by several manufacturers and are often generically referred to as BiPAP. The only bilevels that can be called BiPAP® are the units patented and registered by one manufacturer.
Bilevels are used primarily at night with a nasal, facial or oral mask, or nasal pillows. The FDA has not approved them for off-label use by people with tracheostomies.
Three modes are available with bilevel ventilators:
-
"S" or spontaneous breathing patterns that are sensed so that the unit switches between prescribed pressures;
-
"T" or timed mode that delivers IPAP and EPAP at a predetermined breathing rate;
-
"S/T" or spontaneous/timed that operates in spontaneous mode, but switches to timed mode (referred to as a backup rate) when breaths are not initiated by the individual.
People with neuromuscular disease should use a bilevel ventilator with a backup rate that can initiate breaths, particularly at night.
The advantages of bilevel ventilators are small size, light weight, lower cost and compensation for interface leaks. The disadvantages include lack of internal batteries, fewer alarms, and inadequate pressures for some people, use of more electricity to operate and discomfort from EPAP.
Examples include BiPAP AVAPS (Philips Respironics Inc.) and VPAP™ III ST-A with iVAPS (S9) (ResMed Corp.)
What is a volume-cycled ventilator?
Volume-cycled ventilators deliver a preset volume of air during inspiration. Volume ventilators can deliver higher volumes and pressures than bilevel units, although the volume remains constant despite leaks. The pressure limit can be adjusted by increasing the volume and lowering the high-pressure alarm.
Volume-cycled ventilators can be used for breath stacking (adding one breath to another without exhaling) to enable deeper breaths for improved cough. They also have multiple alarms and internal batteries, but they are larger, heavier and more expensive than bilevel units, although they generally use less electricity to operate. If an individual needs 24-hour ventilation, a volume ventilator is recommended because it is approved by the FDA for this purpose and has the needed safety features.
Examples include LTV® 1100 (CareFusion BD) and the UniVent™ Eagle™ 754 (ZOLL). The popular volume ventilators PLV®-100 (Respironics Inc.) and LP10 (Puritan Bennett) have been discontinued.
What is a pressure support ventilator?
Pressure support ventilators supplement the inspiratory effort of individuals who can breathe spontaneously by providing a preset amount of positive airway pressure throughout the complete inspiration. The tidal volume can vary from breath to breath. These ventilators also offer pressure control with the ventilator rather than the individual controlling the breathing rate.
Examples include Stellar™ 100, Stellar™ 150 (ResMed Corp.) and Vivo® 30, Vivo®40 (Breas).
What is a multi-mode ventilator?
The latest generation of ventilators, multi-mode, can provide many modes of ventilation, such as pressure support, pressure control, volume control, assist/control, SIMV (synchronized intermittent mandatory ventilation), bilevel pressure or CPAP.
Examples include LTV® series (CareFusion BD), HT50®, HT70, HT70+ (Newport Medical Instruments, a division of Covidien), iVent 201® (GE Healthcare), Trilogy 100, 200, 202 (Philips Respironics Inc).
What about ventilators for infants and children?
The choice of a ventilation system in infants and children involves several factors such as the child's age; degree of respiratory impairment; need for positive end expiratory pressure (PEEP), pressure support and higher respiratory rates; and the resources and support systems at home.

Courtesy of Bela Florentin, VACC Camp Coordintor, Miami
Infants who are born prematurely often need a ventilator to help them breathe while in the Neonatal Intensive Care Unit (NICU). Others may have progressive and severe muscle weakness or severe aspiration that caused lung injury. These children usually require a tracheostomy to establish an artificial airway and to protect their developing airways.
Children's ventilatory needs can vary from full respiratory support to partial respiratory support with some ventilator-free time. In children who can initiate a breath and only require night-time support, the use of noninvasive ventilation is increasing. Popular ventilators for pediatric use in the USA include Trilogy, LTV® series and the Newport HT devices. In many developing countries, bilevel ventilators are often the only ventilators that are affordable and available for use.
What is a pneumobelt?
The pneumobelt, also known as an exsufflation belt, consists of an air bag or bladder inside a cloth corset that is worn around the abdomen and lower chest. The pneumobelt is connected by tubing to a positive pressure ventilator that alternatively inflates and deflates the bladder.
As the belt inflates, the abdominal contents are compressed and the abdomen rises, forcing air out of the lungs. When the belt deflates, the diaphragm is lowered and inhalation occurs passively. Because the pneumobelt works with gravity, it is most effective in the sitting and standing positions (at 45° and 90° angles) and cannot be used at night in the supine position.
What is frogbreathing?
Many polio survivors learned to augment their breathing – without a ventilator – by frog breathing or glossopharyngeal breathing. Frog breathing uses the muscles of the tongue, soft palate, pharynx and larynx to force air into the lungs in a repetitive motion. However all the muscles

of the tongue and throat must be functional. Frog breathing requires time and effort to learn, but once learned it can increase the amount of air in the lungs (known as vital capacity), improve cough, stretch the chest, provide better and louder speech, and can provide a person more ventilator-free time.
Which method and ventilator should be used?
The choice of ventilator can be made by your primary physician, or your primary physician may refer you to a pulmonologist (also known as a respirologist) who specializes in breathing-related disorders and lung conditions, and often sleep medicine. Some physical medicine and rehabilitation physicians, known as physiatrists, and some neurologists may also specialize in breathing disorders. In some countries only a pulmonologist can prescribe a ventilator.
After careful evaluation and pulmonary function tests to assess breathing and lung function and capacity (and sometimes a sleep study), the physician recommends a type of ventilator and appropriate interfaces. Individuals who need to use ventilation only at night have different equipment requirements than those who need to use a ventilator around the clock. Sometimes an individual may not be comfortable with a specific ventilator or interface and may need to change the ventilator or interfaces in order to find the most comfortable and effective system.
Some ventilator users combine different methods and ventilators and alternate them, such as using mouthpiece intermittent positive pressure ventilation during the day, augmented by frog breathing and then a nasal mask at night.
How do I obtain the equipment?
The physician writes a prescription that you present to a home health care or medical equipment company. In the USA, physicians work with respiratory therapists in home health care companies that provide the equipment, supplies, and education, training and monitoring. In many countries, respiratory therapy has not developed as a recognized and licensed profession as it has in the USA. Instead, physical therapists (physiotherapists) and/or nurses may assume these tasks. Some large medical centers may provide home health care and education and training in the use of the ventilator at home.
Who pays for the equipment?
In the USA, private insurance carriers generally reimburse for the equipment and related supplies according to their policies, as do Medicare and Medicaid. In countries with universal health care, the ventilator and supplies are usually supplied for free. Other countries have developed systems to cover equipment costs; some also provide personal assistance/attendant care.
What if something goes wrong with the ventilator?
Ventilator users and their caregivers must be prepared for equipment failure, disconnects and power outages, especially if using 24-hour MV, in which case a backup ventilator is prudent. Practicing regular safety drills helps prepare for emergencies. Keeping a manual resuscitator, such as an Ambu® bag, handy at all times is strongly advised.
Will I need specialized care? Can I live at home?

This depends on the medical diagnosis that necessitated the use of MV, and also whether you use MV fulltime. Many part-time and full-time ventilator users live independently. Some people with progressive neuro-muscular diseases may require nurses or attendants/personal assistants who can be trained in the use of the equipment and secretion removal techniques. Children who use 24-hour MV often need nurses to assist their parents in their care.
People who use long-term MV generally prefer to live at home with their families, and many do. They go to school and work; they travel; they participate in their communities; and many rate their quality of life as high. However, if the needed resources cannot be arranged for home care, some long-term ventilator users are placed in skilled nursing facilities.
Where can I find more information?
IVUN's Resource Directory for Ventilator-Assisted Living identifies health professionals and ventilator users who are knowledgeable about long-term ventilator use, ventilator equipment and interface manufacturers, and health organizations.
Many organizations such as The ALS Association, The Muscular Dystrophy Association, The Parent Project for Muscular Dystrophy, Families of SMA and CCHS Family Network provide information on their websites, publish handbooks and guides, and distribute videos on ventilator-assisted living. The ventilator equipment and mask manufacturers provide product information and specifications on their websites.
The 2005 version, Information about Ventilator-Assisted Living, was supported by a bequest from ventilator user Ira Holland, with special acknowledgment to Judith R. Fischer, MSLS, and the late Lisa S. Krivickas, MD, and E.A. Oppenheimer, MD, FACP, FCCP.
2015 update by Joan L. Headley.