IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
VENTILATOR-ASSISTED LIVING
This issue sponsored by:

VOLUME 31, NUMBER 1
FEBRUARY 2017
Dr. Keens, with 39 years of experience, asked, “If chronic respiratory failure means the child is ventilator dependent, why even talk about weaning? How do you wean children from chronic ventilatory support?”
First of all, not all children on home mechanical ventilation can be weaned. Those with fixed or progressive ventilatory muscle weakness are on the ventilator because their muscles are not strong enough to perform the work of breathing. Therefore, unless they have one of the rarer conditions where ventilatory muscle strength can increase, they will not be able to wean........MORE
In 2016, Post-Polio Health International, including the International Ventilator Users Network, Research Fund awarded $100,000 to Louise Rose RN, MN, PhD and Mika L. Nonoyama RRT, PhD, and several supporting team members for the study, CoughAssist: use education needs, health service utilization, and outcomes............MORE
ADDITIONAL SECTIONS
Ventilator Users Speak
Answer questions; learn from others.
Camps for Ventilator-Assisted Children - 2017
Advocacy
Educate, discuss, take action.
Networking
Sharing the work of others.
Recent Relevant Publications
Summaries, links to selected professional, disability, disease journals and newsletters.
Educational Opportunities
Conferences and webinars for health professionals and ventilator users.
Industry
The business of living with a ventilator.
Supported by:
Ventilator-Assisted Living
Vol. 31, No. 1, February 2017
Editor: Joan L. Headley
Designer: Brian Tiburzi
ISSN 1066-534X
© 2017 Post-Polio Health International.
Permission to reprint must be obtained from Post-Polio Health International (PHI) at info@post-polio.org.
Ventilator users, health professionals, non-profits, company representatives – send comments and updates to info@ventusers.org.
Can We Wean HMV Children?

Thomas G. Keens, MD, Division of Pediatric Pulmonology and Sleep Medicine, and Professor of Pediatrics, Physiology and Biophysics at the Keck School of Medicine at the University of Southern California, Los Angeles, California
From Unsung Heroes: Children on Home Mechanical Ventilation, Margaret Pfrommer Endowed Memorial Lecture in Home-Based Mechanical Ventilation, CHEST, October 2016. IVUN previously published "Dr. Thomas G. Keens, Children’s Hospital Los Angeles (CHLA), presents the Pfrommer Lecture at CHEST 2016" in Volume 30, Number 6.
Dr. Keens, with 39 years of experience, asked, “If chronic respiratory failure means the child is ventilator dependent, why even talk about weaning? How do you wean children from chronic ventilatory support?”
First of all, not all children on home mechanical ventilation can be weaned. Those with fixed or progressive ventilatory muscle weakness are on the ventilator because their muscles are not strong enough to perform the work of breathing. Therefore, unless they have one of the rarer conditions where ventilatory muscle strength can increase, they will not be able to wean.
However, in our experience at least 50% of children on home ventilators because of severe lung disease can ultimately be weaned. This is because many of these lung diseases get better with time, and at the same time the child’s respiratory muscles improve in strength. So, you need to select the right patients. But, for some children, weaning from home mechanical ventilation is a realistic goal.
Second, things take time. And, there are limitations. We do not use techniques used in the pediatric intensive care unit.
Parents at home cannot assess responses to a decreased ventilator rate or PIP (peak inspiratory pressure). However, parents can assess if a child tolerates time off the ventilator.
Our approach is “sprint” weaning. We take a child off the ventilator for increasing lengths of time in the home and ask the parents to observe their child and report to us.
“Sprint” weaning also provides ventilatory muscle training. As each sprint increases in length, the ventilatory muscles must gradually perform increasing work of breathing. This is very much the way you would train for a marathon. You start by running a short distance, and gradually increase your distance. Similarly, we start with short sprints, and gradually increase the time the child is doing the work of breathing.
Our procedure is to slowly increase “sprint time” as tolerated.
No one, not even an adult, breathes as well during sleep as while awake. Thus, we wean first while awake and only wean from sleep once off the ventilator while awake.
This approach permits ventilator-free time at home during the day, which is good for family activities. Time off the vent during the day allows us to clinically assess the tolerance for weaning by visiting the home.
Periodically, we evaluate objectively the tolerance for weaning in the clinic with checks of SaO2 and PetCO2. If the numbers are good, we slowly advance the time off the vent while awake.
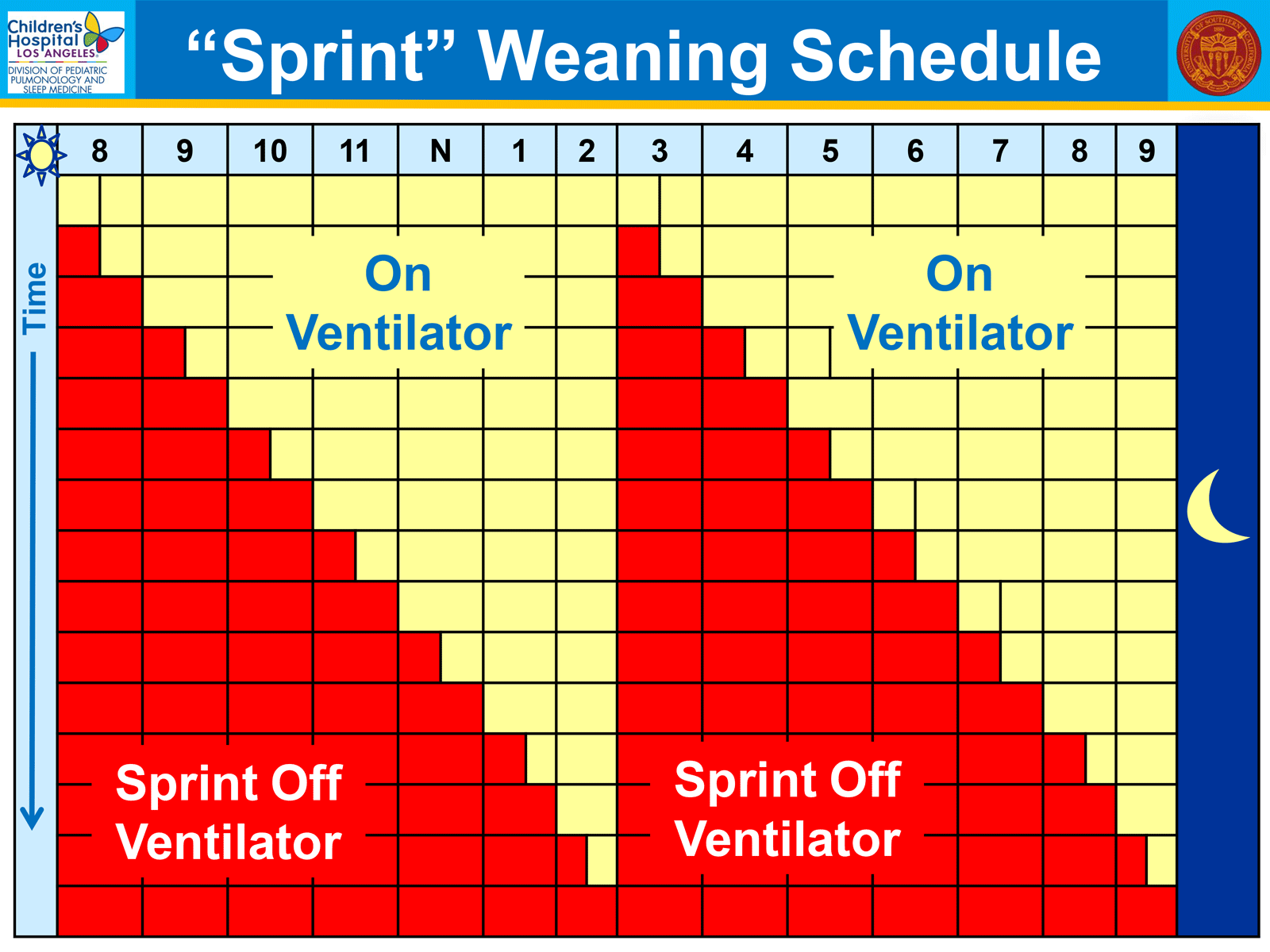
We know that the time to wean will be slower at home than in the hospital with close observation, and we consciously avoid the temptation to go too fast.
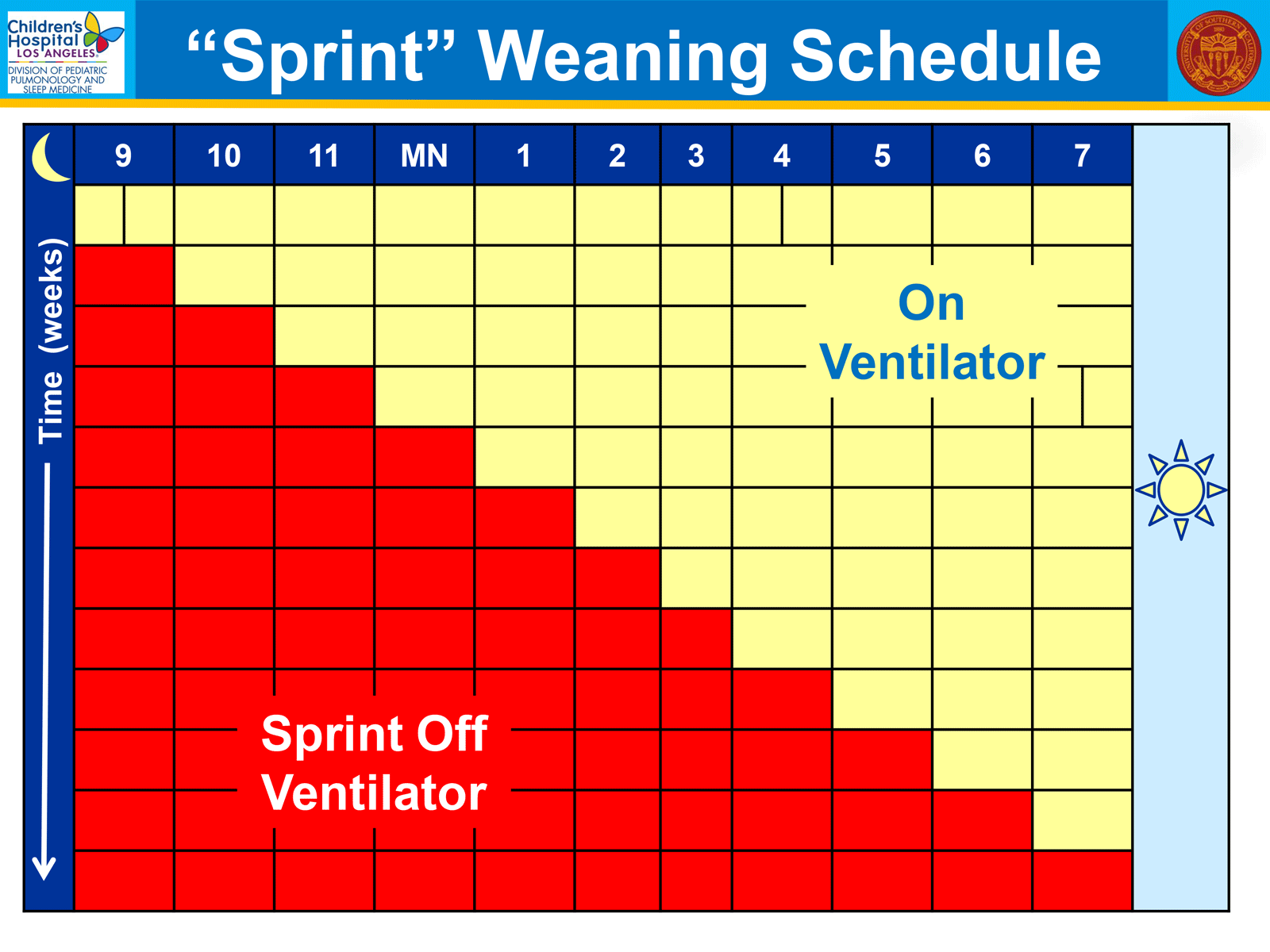
Once off the ventilator at all times while awake, we will wait a period of time to confirm its success.
Next, we perform an overnight polysomnogram with spontaneous breathing. If PetCO2 <50 torr, we begin weaning at night. Knowing we need to go slowly, we increase sprint time asleep by one-hour per week.
Weaning is not always successful. These are the signs we look for that indicate weaning failure.
-
Rising PetCO2 and the need to return to the ventilator.
-
Frequent and/or severe pneumonias.
-
Growth failure (caloric expenditure due to work of breathing).
-
Energy available for activities which enhance quality of life.
In summary, some children can be weaned from ventilatory support. However, you have to have patience. It is a slow process. We perform weaning using “sprint weaning,” so parents can monitor the progress of their children at home. This process works well and having the families do this weaning empowers them to try other things which improve the quality of the ventilator-assisted child’s and family’s lives.

For more information, refer to Keens, T.G., et al. Rogers’ Textbook of Pediatric Intensive Care. 2015. pp 794-807.
PHI/IVUN Research Update
In 2016, Post-Polio Health International, including the International Ventilator Users Network, Research Fund awarded $100,000 to Louise Rose RN, MN, PhD and Mika L. Nonoyama RRT, PhD, and several supporting team members for the study, CoughAssist: use education needs, health service utilization, and outcomes. (See Organization Awards $100,000 for Study in 2016-2017)
This study, designed to be conducted over two years, aims to better understand CoughAssist (Philips Respironics) user needs for initial and ongoing education and support as well as barriers and facilitators to initial use of the CoughAssist device using telephone interviews of users and caregivers.


Louise Rose, RN, MN, PhD
Mika L. Nonoyama, RRT, PhD
Additionally, the study aims to conduct a longitudinal study to evaluate the impact of the Canadian government funded CoughAssist Program on the following: health service utilization including emergency department visits and hospital admissions, patient outcomes such as health related quality of life and symptom management, and peak cough flow, as well as to document user compliance with their CoughAssist device prescription.
The lead researchers report, "After completing research ethics board requirements we have been successful in recruiting experienced users and experienced caregivers as well as new users and new caregivers to participate in telephone interviews. The data collection phase of this part of the study is therefore nearing completion and we will commence analysis of the interview transcripts in the coming months.
"We have experienced some challenges in the recruitment of study participants for our longitudinal study evaluating the impact of the CoughAssist program on healthcare utilization, health related quality of life and symptoms. Our new research officer is now based at the Ventilator Equipment Pool in Ontario and is actively recruiting participants."
Ventilator Users Speak
Cataract Surgery for a Ventilator User
Dave Marven, Oshawa, Ontario
Like many seniors, as I aged my vision gradually lost sharpness and colour perception. At 79, the natural lenses in my eyes were cloudy enough to be replaced (cataracts). The surgery is less than 10 minutes.
But would using a ventilator and a mask present challenges?
The Ventilation Equipment Pool in Ontario, which provides and maintains equipment for about 8,000 qualified users, had limited information to assist. However, with today's modern equipment, more ventilator users are now reaching the age when cataracts may develop. A plan is important.
For my Oshawa team (ophthalmologist and anesthetist), I was their first vent patient. For my cataract surgery, the surgeon preferred me lying down and not using a mask. So, I switched my Trilogy 200 (Philips Respironics) to Mouth Piece Ventilation (MPV).
Things went really well. They placed the Trilogy at my feet and attached a 6-foot hose with MPV tubing at the end. I held the tubing in my hand close to my mouth. I was placed on my back and propped comfortably with pillows in the correct position.
They froze my eye but gave me no sedation. That way, I had full control of my breathing and was alert to turn my head, etc., on instruction. The surgeon was very pleased. Perfect conditions from his viewpoint.
As for me, I had no discomfort at all. It was easier than a dental cleaning.
Before surgery, I had to decide the type of lens to replace my natural ones. Most non-ventilator users pick distant lenses and wear reading glasses for things close up. But for me, it would be difficult to wear glasses when I wanted to use my vented mask at the same time.
For my first surgery on the left eye, I chose the Abbott Multi Focus ZMT300 (M.F.). It is designed to work with an M.F. in the right eye to help provide freedom from glasses by giving both near and distant vision. There is an extra cost to this lens option, which is available in Canada.
Two months later, however, I do not as yet have satisfactory close vision from the M.F. in the left eye. It will take more time, I understand. As a result, I will decide later what to do with the right eye.
I would like to hear about the experiences of other ventilator users with cataract surgery. Has anyone had their surgery done sitting up? What procedure and what replacement lenses worked for you? We can learn from each other. Contact me at info@ventusers.org or at dmarven@aol.com.
For general information: Considering cataract surgery? What you should know.
Ventilator users respond to question about backup generators
Andrea asks: “I want to purchase a generator for my mom's vent. I need to know do most folks use a portable or has anyone ever gone all in and gotten one for the whole house? If anyone can recommend brands that would very helpful.”
Charlie responds: “I have a Honda EU3000, which supplies 3000 watts. We have a transfer switch that switches out the circuits that I need to run most of my house. When I use the generator, it powers everything except the high wattage equipment. Things like the oven, dryer, air-conditioner are not powered by the generator. For us, this is a whole house solution. However, if you want to power just the ventilator and aspirator, you don't need this much wattage. A small Honda generator would supply power for lifesaving equipment.”
Jim responds: “We have a Honda EU2000i generator. It's a 2000 watt portable. It works great to power essentials during an outage.
“We have the ventilator (Trilogy 100), humidifier, suction machine, bed and air mattress plugged into a Tripp Lite 8 Outlet Industrial Safety Surge Protector Power Strip with 25-foot Cord, which is plugged into house wall power.
“During a power outage, we pull the generator outside, unplug the power strip from the wall socket, run the cord out the window to the generator. This is not as convenient as a transfer switch, but it works for us at little cost.
“However, we recently purchased a Champion DUAL-FUEL 2800 wt Running/3100wt Peak Digital Inverter Generator, Electric Start from Costco. I have not had a chance to try it yet. We got this one since it can run on gasoline or liquid propane (like we use with the grill). The LP tanks can be safely stored where the gasoline needs to be replaced since it goes bad.
“I am on a Trilogy 100 ventilator and we have the Respironics Trilogy External Battery Cable (Model 1047295) connected to a deep-cycle battery. The ventilator automatically switches to the external battery when it loses AC power. It last longer than the internal batteries. The battery is also connected to a Battery Buddy Intelligent 6V/12V Battery Charger/Maintainer.”
Eric responds: “I have a 6000 watt Generac generator. It plugs into a special socket in my attached garage. It gets cold in Wisconsin so the generator is wired to the furnace, sump pump, refrigerator, microwave and my entire room.
“If I had to do it over again, I would definitely do the whole home solution, and I'll tell you why.
“I was once without power for three days and had to survive on a little 1200 watt camping generator. My poor dad had to run those long orange extension cords into the house and rotate them between the refrigerator, sump pump, etc. Anytime one of those appliances would kick in, the generator would struggle. (The Generac is rated for 12,500 "surge watts.")
“The whole home solutions are really sweet. They run on LP gas and come on automatically whenever power is lost. If you don't have a lot of money, the camping generator will do in a pinch. Just run it occasionally (at least once a month).”
One ventilator user's struggle with persistent infection
Peg reports, “My health is quite good now, but the first half of the year was a bit difficult. Since November 2015 I had been dealing with a persistent infection in the tracheostomy where I attached the breathing machine. Amazingly, it disappeared this past June after my weekend attendant quit. Now, I am super cautious about how people lift me so that they avoid pulling on the tubes. The doctors say the bug still shows up on blood tests, but I am symptom-free. Lesson: my new attendants need excessive and very careful training. Chest pains propelled me to the ER last January and it took 4½ days of testing for them to tell me they couldn’t find anything wrong. I guess that’s good, right? Lesson: stay away from hospitals!”

Questions for ventilator users and health professionals, too
My name is Patrick (pcho@bcits.org), and I am one of the Respiratory Therapists working for the Provincial Respiratory Outreach Program in British Columbia, Canada. We are reaching out to other vent user communities to get some perspective on cuffed trach management.
We provide respiratory services for those clients that qualify for our program and one of those criteria is a having a cuffless trach tube. We feel that a cuffed client generally is less stable and require more support than what our community resource can provide. They end up going to facilities or try to wean to a cuffless trach.
-
In your perspective and experience, do you see many cuffed trach tubes living the community?
-
Who is providing the education for them?
-
Who is managing the cuffed trach tube, nurses, family, private caregivers?
-
Any common issues or ongoing problems that cuffed trach tube users encounter?
Patrick Cho, BSc, Registered Respiratory Therapist pcho@bcits.org
Camps for Ventilator-Assisted Children - 2017
CAMP PELICAN
Camp Pelican, the New Orleans area, hosts a week-long overnight resident camp for children with pulmonary disorders-such as but not limited to severe asthma, cystic fibrosis, tracheotomy and ventilator assisted children. Camp Pelican will be May 28-June 3, 2017. Camper and Staff Applications are available March 15, 2017.
The 2017 VACC Camp will take place April 8-14.
VACC CAMP
PA Vent Camp is held annually at Camp Victory in Millville, PA. June 25-30 are this year’s dates.
PA VENT CAMP
CAMP INSPIRATION
Camp Inspiration is specifically for BiPAP and ventilator-assisted children at Double H Ranch, Lake Luzerne, New York. June 6-10 are the dates for 2017.
FRESH AIR CAMP
Fresh Air Camp is scheduled for June 11-16, 2017 at Camp Cheerful, Strongsville, Ohio.
CHAMP CAMP
CHAMP Camp 2017 will be June 18-22, 2017 at Bradford Woods, Martinsville, Indiana. Counselors may apply here. Campers can apply here. All applications are due by March 1, 2017. Make sure to get in on time, and we hope to see you at camp! If you have any questions, please call 317-679-1860 or send an email to jennifer@champcamp.org.
VICTORY JUNCTION
Victory Junction enriches the lives of children with chronic medical conditions or serious illnesses by providing life-changing camp experiences that are exciting, fun and empowering; all in a medically-safe environment at no cost to the camper or their family.
Located in the hills of Randleman, North Carolina, Victory Junction is spread across 84 acres, allowing children to do what they do best— be kids, play, imagine, make friends and enjoy the adventures and experiences of camp life.
Ashley Seeley, MPA, at Victory Junction explains that they do not have a special weekfor children who use vents, but they do have Specialty Weekend in August which is a perfect opportunity for children to come out and experience camp with their families. The weekend long session at the end of summer happens when activities are still going on (waterpark, ropes course, etc.)
“I think that it would be a perfect opportunity for your families to apply. We serve children 6-22 within that session. Again, it’s a family session and they would all attend camp together. This year, our Specialty Weekend is August 11-13 (Fri-Sun).”
Check out the Application Guides for Family Weekend.
TRAIL'S EDGE CAMP
Trail’s Edge Camp is a week long summer camp for children who are ventilator-assisted. 2017's camp will be held June 4-9 at the Fowler Center for Outdoor Learning, a beautiful barrier-free camp on 200 acres in Mayville, Michigan.
Advocacy
Christopher & Dana Reeve Foundation
Christopher & Dana Reeve Foundation invites all individuals with paralysis to Advocate for Change.
Resources regarding possible changes to healthcare
Families USA Foundation is a nonprofit, nonpartisan, 501(c)3 organization, founded in 1981, that has served the healthcare movement for more than 30 years. It is headquartered in Washington, DC. They are working to be sure there is a replacement of the ACA before repeal. They have developed comprehensive facts sheets, talking points, etc. Check them out.
There has been a lot of discussion about block grants. Block grants are “bad." Block grants are “good.” Here is a New York Times article that asks, How Would Republican Plans for Medicaid Block Grants Actually Work?
Update on contact with CMS regarding coverage of RADS and vents
NAMDRC (National Association for Medical Direction of Respiratory Care) reports that after the election they had to regroup but it is working with Congressman Chris Collins (R-NY), who is a member of the House Energy & Commerce Committee. Meetings are scheduled “on the Hill” this week.
Recent news regarding IDEA
The US Department of Education includes the Office of Special Education and Rehabilitative Services (OSERS), which includes the Office of Special Education Programs (OSEP). OSEP is dedicated to improving results for infants, toddlers, children and youth with disabilities ages birth through 21 by providing leadership and financial support to assist states and local districts.
Basic to the lives of children and youth with disabilities is the Individuals with Disabilities Education Act of 2004 (IDEA). Parents and disability advocates took note that during questioning at the confirmation hearings for Betsy DeVos (now Secretary of Education) her responses about IDEA (a federal law) showed a lack of understanding about the rights and needs of children and youth with disabilities.
The website for IDEA, which disappeared, has now been restored. The site states, “After a technical outage of this page, the Office of Special Education and Rehabilitative Services (OSERS) has restored the functionality and resources that were available prior to February 8, 2017.”
Advocates are simultaneously watching the Department of Education’s actions and offering their extensive experience and advice to the new leadership.
Networking
Google honors disability rights pioneer Ed Roberts
On January 23, 2017, Google Doodle marked what would have been the 78th birthday of Ed Roberts. He is considered by many the father of the independent living movement and a pioneer in disability rights and civil rights. A childhood polio survivor, his activism started in high school, where he successfully advocated for school administrators to remove driver education and physical education requirements so he could graduate. As a college student, he co-founded the Physically Disabled Students Program at the University of California, Berkeley, the first program of its kind. Under his leadership, the Berkeley Center for Independent Living became a model for disability rights movements around the world. Ed Roberts received a MacArthur Foundation "Genius Grant" and used it to establish the World Institute on Disability (WID) in Berkeley.
Got Transition
Got Transition/Center for Health Care Transition Improvement is a cooperative agreement between the Maternal and Child Health Bureau and The National Alliance to Advance Adolescent Health.
Their aim is to improve transition from pediatric to adult health care through the use of new and innovative strategies for health professionals and youth and families. With a broad range of partners, they are working to:
-
Expand the use of the Six Core Elements of Health Care Transition in pediatric, family medicine, and internal medicine practices;
-
Partner with health professional training programs to improve knowledge and competencies in providing effective health care transition supports to youth, young adults, and families;
-
Develop youth and parent leadership in advocating for needed transition supports and participating in transition quality improvement efforts;
-
Promote health system measurement, performance, and payment policies aligned with the Six Core Elements of Health Care Transition; and
-
Serve as a clearinghouse for current transition information, tools, and resources.

Contact Information
Got Transition
1615 M Street NW, Suite 290
Washington, DC 20036
202-223-1500, 202-429-3957 fax
info@GotTransition.org, www.GotTransition.org
From the Social Security Administration
Getting to Know the ABLE Act
The above links to several Q&As, e.g., Do I have to wait for my state to establish a program before opening an ABLE account?
No. Regardless of where you might live and whether your state has decided to establish an ABLE program, you are free to enroll in any state’s program, if the program accepts out-of-state residents.
For more in-depth information about the ABLE Act and ABLE programs, including which states offer enrollment, please visit the ABLE National Resource Center.
From Agency for Toxic Substances and Disease Registry (ATSDR)
National ALS Biorepository
The National Amyotrophic Lateral Sclerosis (ALS) Biorepository is here! To take part you will need to join the National ALS Registry and agree to learn more about the Biorepository. If you have already joined the Registry you will need to log into your account and update it to get more information about the Biorepository.
Visit the Biorepository webpage to learn more.
Two young entrepreneurs win part of the ALS Assistive Technology Challenge
December 20, 2016 - Dexter Ang was inspired to get involved with assistive technology after caring for his mother who had ALS. He and his business partner, David Cipoletta, and their company, Pison Technology, were awarded one of the prizes from The ALS Assistive Technology Challenge, sponsored by The ALS Association and Prize for Life. They blew the judges away with their easy-to-use, self-contained communication system based on muscle EMG signals. People living with ALS are able to learn and use the system to communicate in minutes. Learn more about these two young entrepreneurs and their exciting new technology on their blog.
CHEST Foundation
The CHEST Foundation creates trusted patient education resources and disease awareness campaigns that empower patients to engage in better managing their health. Check out their Patient Education Resources.
Recent Relevant Publications
From CHEST Physician
“Disease-modifying medications may soon become ‘game changers’ in many neuromuscular conditions. However, a significant concern is the expected prohibitive cost….”
Home-Based Mechanical Ventilation and Neuromuscular Disease Update: Advances in neuromuscular disease in CHEST Physician, Vol. 12, No. 2, February 2017 by Ahlam Mazi, MBBS, Fellow-in-Training.
Home, community based services work
Mathew C. Schwarz. The Bismark Tribune. Jan 11, 2017.
“As a parent with a child who has severe disabilities, including the use of a ventilator, tracheostomy, continuous oxygen, etc., home and local support services work very well if adequate resources are provided. Our family has proven that it works for almost 30 years.” Read full article.
From Journal of Neurology, Neurosurgery, & Psychiatry
“These data confirm that NIV improves survival in MND/ALS. The overall magnitude of benefit is 13 months and was largest in those with ALS-bulbar disease. Future research should explore the optimal timing of NIV initiation within phenotypes in order to optimise respiratory function, quality of life and survival.”
Identifying who will benefit from non-invasive ventilation in amyotrophic lateral sclerosis/motor neurone disease in a clinical cohort by David J Berlowitz, et.al. in J Neurol Neurosurg Psychiatry, Volume 87, Issue 3, March 2016. Correspondence to David J Berlowitz, Institute for Breathing and Sleep, Bowen Centre, Austin Hospital, Studley Rd, Heidelberg, VIC 3084, Australia; david.berlowitz@austin.org.au.
“We describe the importance of NIV failure due to upper airway obstructive events, the clinical characteristics, as well as their impact on the prognosis of ALS.”
Research paper: Reduced survival in patients with ALS with upper airway obstructive events on non-invasive ventilation by Marjolaine Georges, J Neurol Neurosurg Psychiatry, Volume 87, Issue 10, October 2016. Correspondence to Jesus Gonzalez-Bermejo, Département “R3S”, Service de Pneumologie et Réanimation Médicale, AP-HP, Groupe Hospitalier Pitié-Salpêtrière Charles Foix, 47-84 Bd de l'hopital, Paris 75651, Cedex 13, France; jesus.gonzalez@aphp.fr.
From HealthDay
"These time-consuming and sometimes technical health care tasks can include maintaining ventilators, performing physical therapy, tracking medication and changing bandages. Guaranteed paid sick leave or family leave also would help, by removing the financial stress that can come from missing work to care for a chronically ill child."
U.S. Families Spend 1.5 Billion Hours Yearly on Kids with Special Health Needs (December 27, 2016)
From the Food & Drug Administration
FDA approves drug to treat Duchenne muscular dystrophy (Emflaza is a corticosteroid that works by decreasing inflammation and reducing the activity of the immune system. Emflaza is marketed by Marathon Pharmaceuticals of Northbrook, Illinois. After a pricing increase was revealed the company posted An Open Letter to the Duchenne Community, that includes, “We are pausing our commercialization efforts…”
“First, rinse only with distilled, sterile or previously boiled water. Tap water isn’t safe for use as a nasal rinse because it’s not adequately filtered or treated.”
Is Rinsing Your Sinuses With Neti Pots Safe? (January 24, 2017)
From CureSMA.org
“All individuals affected by SMA have at least one copy of survival motor neuron gene 2 (SMN2), often referred to as the SMA "backup gene." Due to a splicing error, most of the SMN protein made by SMN2 is missing an important piece, called exon 7. Antisense drugs are small snippets of synthetic genetic material that bind to ribonucleic acid (RNA), so they can be used to fix splicing errors in genes such as SMN2. Spinraza is antisense oligonucleotide that targets SMN2, causing it to make more complete SMN protein.
“Spinraza was first known as IONIS-SMNRx, then nusinersen.”
From The Lancet United States of Health Blog
“Last June, California became the fifth state (Colorado is now the sixth) to allow terminally ill patients to request and obtain a lethal prescription, which they take home and ingest, thereby ending their suffering by ending their lives.
“The legal mechanism is complicated, with safeguards such as consent from two physicians and a 15-day waiting period, designed to prevent ethical abuses.”
Berkeley Doctor Wants to Help California Patients, Hospices with Aid-in-Dying Law (February 1, 2017)
From Not Dead Yet
“On November 11, 2016, NDY sent a letter to the AMA, the first of two submissions urging the AMA through its Council on Ethical and Judicial Affairs to re-affirm its position opposing legalization of assisted suicide.”
NDY Urges AMA To Affirm Longstanding Opposition to Legalizing Assisted Suicide
Educational Opportunities
FOCUS Spring 2017
May 5 - 6, 2017, Friday, Saturday, with additional optional workshops on May 7th, Sunday morning, Rosen Shingle Creek Resort in Orlando, Florida. Watch for details.
Parent Project Muscular Dystrophy 2017 Annual Connect Conference
June 29 to July 2, 2017, Chicago, Illinois. Save the date.
European Respiratory Society (ERS) International Congress 2017
September 9-13, 2017, Milan, Italy. Registration will open in April 2017 from this website.
CHEST 2017
October 28- November 1, 2017, Toronto, Canada. Submit an abstract of your original investigative work or a case report. Submissions are due March 31. Learn more and submit.
JIVD/ERCA Conference in 2018

First announcement: JIVD (Journes Internationales de Ventilation Domicile) and ERCA (European Respiratory Care Association) are working on the organization of their third joint meeting that will take place in Lyon, France, March 15 - 17, 2018.
CCHS Family Conference 2018, alongside The 5th International CCHS Conference
June 19-23, 2018 at The Chase Park Plaza, St. Louis, Missouri, USA.
Industry
Utah County doctor's invention could save thousands of lives
“The two men are primaries at the neonatal department at Utah Valley Regional Medical Center in Provo. The men have worked for years in developing nations and saw a need for a ventilator that rural clinics in countries like Cambodia could afford.” More.
Chris Jones, KUTV, Salt Lake City, Feb 2, 2017.
University of Michigan's AIM Tech creates low-cost ventilator for developing nations
“The problem: Every year more than one million babies die of respiratory illnesses, most in low-to-middle-income countries. The solution: an affordable, high quality, low-tech pressure ventilator.”
AIM Tech, of the University of Michigan, created a ventilator to help children in developing countries. The creators won the 2017 Cardinal Challenge business plan contest in Louisville, Kentucky. NeoVent costs less than 1/100th the price of existing ventilators, the team says, is easy to use and requires no electrical power. AIM Tech won $15,000 cash and a $100,000 Launch in Louisville incentive of in-kind services, provided the company locates in Louisville.
From the Food and Drug Administration
This means manufacturers should, among other things:
-
Have a way to monitor and detect cybersecurity vulnerabilities in their devices
-
Understand, assess and detect the level of risk a vulnerability poses to patient safety
-
Establish a process for working with cybersecurity researchers and other stakeholders to receive information about potential vulnerabilities (known as a “coordinated vulnerability disclosure policy”)
-
Deploy mitigations (e.g., software patches) to address cybersecurity issues early, before they can be exploited and cause harm










