IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
IVUN
INTERNATIONAL VENTILATOR USERS NETWORK
an affiliate of Post-Polio Health International
CONNECTING
VENTILATOR USERS,
HEALTH PROFESSIONALS,
AND INDUSTRY
VENTILATOR-ASSISTED LIVING
This issue sponsored by:

VOLUME 29, NUMBER 5
OCTOBER 2015
NICOLAS MEYERING, DENTON, TEXAS
I have a lifelong condition called congenital central hypoventilation syndrome (CCHS), which is a nervous system disorder that means I don’t automatically breathe when I’m asleep. Growing up with a rare disorder taught me about the importance of monitoring my health and helping others.
During my undergraduate years at Hartwick College, Oneonta, New York, I became very involved in volunteering. I continued volunteering during my graduate education at Binghamton University, Binghamton, New York........MORE
DEBORAH GRAYSON CARPENTER, HOUSTON, TEXAS
I was diagnosed with Spinal Muscular Atrophy Type 1 on my first birthday. My life expectancy was 2 years old. Growing up, I had three brothers and received no special treatment. My mom always said, “Don’t let people tell you that you can’t. You just do it differently.”
Today, I’m 47 years old. I’m in a wheelchair and have scoliosis........MORE
ADDITIONAL SECTIONS
CHEST NetWork Renamed
Networking
Sharing the work of others.
Advocacy
Educate, discuss, take action.
Ventilator Users Speak
Answer questions; learn from others.
Recent Relevent Publications
Summaries, links to selected professional, disability, disease journals and newsletters.
Educational Opportunities
Conferences and webinars for health professionals and ventilator users.
Industry
The business of living with a ventilator.
Supported by:
Ventilator-Assisted Living
Vol. 29, No. 5, October 2015
Editor: Joan L. Headley
Designer: Brian Tiburzi
ISSN 1066-534X
© 2015 Post-Polio Health International.
Permission to reprint must be obtained from Post-Polio Health International (PHI) at info@post-polio.org.
Ventilator users, health professionals, non-profits, company representatives – send comments and updates to info@ventusers.org.
Goal: Living as Independently as Possible
NICOLAS MEYERING, DENTON, TEXAS
I have a lifelong condition called congenital central hypoventilation syndrome (CCHS), which is a nervous system disorder that means I don’t automatically breathe when I’m asleep. Growing up with a rare disorder taught me about the importance of monitoring my health and helping others.
During my undergraduate years at Hartwick College, Oneonta, New York, I became very involved in volunteering. I continued volunteering during my graduate education at Binghamton University, Binghamton, New York. I helped run a weekly soup kitchen for low-income community members. I helped plan two fundraisers that each raised over $3,000 for local charities. I even got elected to student government and led my classmates in donating over 100 pairs of socks and underwear to victims of Hurricane Sandy.
Before I graduated with my Master’s degree in Public Administration, I was inducted into Sigma Alpha Lambda, an honor society for students who do well in school and focus on public service.

After I graduated, I began taking an active role in the CCHS Family Network*, the nation’s only nonprofit support group for people with my condition. The group began thanks to my mother, Mary Vanderlaan, PhD, and her hard work. It is an honor to help maintain and grow the Network.
I handle parts of the CCHS Family Network’s fundraising, social media and admissions process. It is always a joy to meet new CCHS families and to make friends all over the world.
The Network holds conferences every three to four years. Our next conference is in 2018, and I want to combine my video game hobby with a chance to fundraise for the Network. I’d like to host a 24-hour video game marathon where people can sponsor participants.
I believe that adults with disabilities need to be role models for children with disabilities. I believe that people with disabilities need to be actively involved in advocating for their needs. And, most firmly, I believe that young people with disabilities need to live as independently as possible.
I live in Denton, Texas, which is in the northern part of the state. I handle social media, communications, outreach and public relations for a small human services non-profit called Interfaith Ministries. We provide assistance to people experiencing sudden financial crises.
I love being able to help others in need, because I know that I have always had help getting where I am today.
Getting Ready for Sleep
Each night before bed, I wash my face with baby shampoo to make sure my skin is clean and soft so my face mask (Respironics Total Full Face Mask) won’t irritate my skin.
Using a ventilator (ResMed’s VPAP III ST-A) at night means that I need to keep allergies and nasal congestion under control. I have an over-the-counter nasal spray that I use to keep my breathing passages clear.
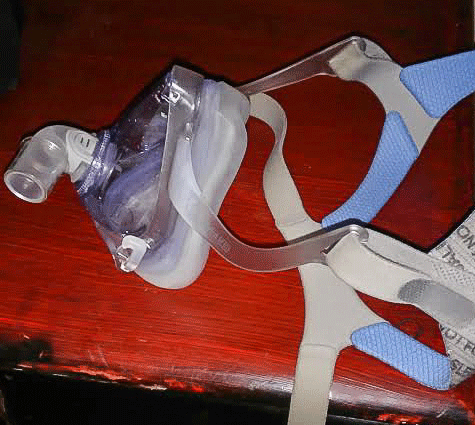
Respironics Total Full Face Mask
I wrap one of my toes in medical tape so the lead from the oximeter does not cause a blister right away. I only use one pillow at night because my vent works best when I am laying down completely. I have written my vent settings on a notepad that I have attached to my bedside table, which is where I place my vent.
Each morning I take omega-3 vitamins which promote heart health. I try to adhere to a heart-healthy diet since some people with CCHS experience cardiac pauses. Thus, I take heart health very seriously. I eat a lot of salmon, salad, strawberries, blueberries, almonds, walnuts, dark beans, carrots and oatmeal. On top of that, I take a daily multivitamin.
Finally, I wash my mask and tubing with a vinegar-water solution once a week.
With a little extra care, there are very few things people with vents cannot do!
*The CCHS Family Network is a non-profit, tax-exempt organization registered in the United States. Its efforts focus primarily on education and support of our families and CCHS patients, inter-family and family-physician communication, and supporting and facilitating CCHS research.
Nico’s Hints for People with Vents
Going to College:
-
If there are times of the day when you are more likely to need your vent, pick classes that don’t meet at those times.
-
If you are sleepy in class, walk around, use the bathroom, get a drink, etc.
-
Make sure your professors and any disability support staff know about your condition, what to do in an emergency, and any special needs or considerations you have.
Living Independently:
-
Make sure your vent settings are written down in plain sight somewhere.
-
If you have roommates or you live with a partner, tell them about your condition and what to do in an emergency.
-
Write down emergency contact information (family, physician, hospital) in plain sight.
-
Live somewhere safe, comfortable and clean. It’s worth it to spend a little more money to live somewhere healthy.
Travel:
-
If your vent is in a carry-on suitcase, wrap it in clothes and soft materials so it doesn’t knock up against something hard and get broken.
-
If traveling at night, make sure you can set up your vent/pacers in your vehicle. I use my pacers (breathing pacers placed near my phrenic nerve from Avery Biomedical) on plane rides and used my vent in the family car when I was a child.
-
If driving, stop frequently for naps, breaks, and general rest.
1953 Ventilation Yields 2015 Fashion
DEBORAH GRAYSON CARPENTER, HOUSTON, TEXAS
I was diagnosed with Spinal Muscular Atrophy Type 1 on my first birthday. My life expectancy was 2 years old. Growing up, I had three brothers and received no special treatment. My mom always said, “Don’t let people tell you that you can’t. You just do it differently.”
Today, I’m 47 years old. I’m in a wheelchair and have scoliosis.
I started sleeping in an iron lung when I was ten years old due to getting pneumonia every year. I firmly believe that I’m still here today because of God, my parents, having an awesome respiratory physician named

Gunyon Harrison, MD, at Texas Children’s Hospital in Houston, Texas. He was the only one who promoted use of the iron lungs. The other physicians used tracheotomies.
I received the lung from TIRR (The Institute for Rehabilitation and Research, now TIRR Memorial Hermann). It was paid for by Muscular Dystrophy Association until they stopped in 2012 due to cut backs.
It was manufactured in 1953, so it is well over sixty years old. Now my husband of 25 years does all the maintenance on it keeping all the moving parts greased, and the leather diaphragm oiled. The best belt is a drive belt for a riding lawnmower blade, the best oil for the leather diaphragm is Baseball Glove Oil, and for grease he uses a good silicone lube. The only part I have replaced lately is the yellow spiral collar.
I have had pneumonia only once and that was when I was 44 years old. I have occasional bouts of bronchitis due to allergies, and the iron lung has kept me out of the hospital each time. I am firmly convinced that it has kept me alive for decades longer than a positive pressure respirator would have.
I use a BiPAP machine when I travel. I wish negative ventilators weren’t so hard to find, because I really need to find a Porta-Lung for travel. The BiPAP doesn’t inflate my upper chest like the iron lung does.
I attended Olson Elementary school for a few years, but after getting pneumonia every year I started home schooling and two teachers came twice a week to my home. I attended high school at McCullough High School from September thru November and March until May each. The rest of the time I was schooled at home due to the risk of flu.
I graduated from high school in 1986 with a four year scholarship awarded to me by my peers. I went to University of Houston for a year, and then to Texas Paralegal where I earned my paralegal certificate. I finally ended up working 16 years at Continental Airlines, now United Airlines.
Currently, I’m pursuing my modeling career. I have appeared in three fashion shows so far. I competed in the Ms. Wheelchair Texas Gala where I received the title Ms. Wheelchair Texas Ambassador. I also am National Spinal Cord of Houston Ambassador.
My most recent achievement was being appointed Brand Ambassador for TeKay Designs by Kimma Wreh, a world renowned award winning designer. Kimma was recently appointed Madam Ambassador for Liberia. Together we plan to make huge contributions to the community, as well as raise awareness for the need for inclusion of models with disabilities in fashion.
For more information, visit my website www.deborahgraysoncarpenter.com.
*Dr. Gunyon Harrison, age 94, is Professor Emeritus, Pediatrics-Pulmonary, Baylor College of Medicine, Houston, Texas.
CHEST (American College of Chest Physicians) NetWork Renamed
Under the leadership of immediate past chair, Lisa Wolfe, MD, FCCP, Northwestern Memorial Hospital, Chicago, Home-Based Mechanical Ventilation and Neuromuscular Disease NetWork is the new name of the Home Care NetWork.

At the NetWork Meeting at CHEST 2015, Dr. Wolfe passed the baton to David Zielinski, MD, FRCPC, Montreal Children’s Hospital, who in turn introduced the new Vice-Chair Howard Panitch, MD, FCCP, director of the Technology Dependence Center at Children's Hospital of Philadelphia (CHOP).
The renamed NetWork is comprised of members who care for patients in the home or who have special interest in promoting the development of home care as a viable alternative to in-hospital care.
Dr. Zielinski stated in CHEST Physician, August 15, 2015, “Today, home-based ventilation is given for a wide variety of diseases, including neuromuscular diseases, chronic lung diseases, central hypoventilation syndromes, spinal cord injuries, and many others. At the same time, support is being increasingly provided with noninvasive ventilation, including up to 24-hour ventilator requirements, and new equipment and skills are being developed on a regular basis to facilitate this support.
“There are also many challenges that accompany this growing population. One priority our steering committee has repeatedly heard is that patients with progressive neuromuscular diseases, especially in adulthood, are having difficulties finding clinicians to provide appropriate noninvasive ventilation. And even when they do and are well cared for, they risk receiving a tracheostomy when they are admitted to hospitals after admissions for acute decompensations, despite experience and literature suggesting this is often avoidable.”
“The activities of the Steering Committee, which meets quarterly via conference call, help raise awareness amongst physicians and healthcare providers regarding the needs and appropriate care of ventilator users,” states Dr. Zielinski. If you would like to be more actively involved contact, zielinski_dave@yahoo.com or info@ventusers.org.
Preceding the NetWork meeting, the Home-Based Mechanical Ventilation and Neuromuscular Disease NetWork Featured Lecture, “Administration of Noninvasive Ventilation Programs,” was presented by Andrea H. S. Loewen, MD, FRCP(C), Alberta Health Services, University of Calgary, Canada.
Dr. Loewen stated that in Calgary sleep and neuromuscular conditions are treated in separate facilities, the funding structure for noninvasive and invasive ventilation is different and with several suppliers of equipment, communication can be problem. She explained that each nurse and respiratory therapist she interacts with regarding a patient has their own other manager in their facility. Dr. Loewen said pragmatically, “Sometimes I feel like the ventilation program only exists in my mind.”
Recently, the program has made prompt and accurate communication a priority with positive results.
Also at CHEST 2015, Dr. John R. Bach, MD, presented the Margaret Pfrommer Memorial Lecture in Long-term Mechanical Ventilation at CHEST 2015. See next Ventilator-Assisted Living (Volume 29, Number 6) for more details.
Joan L. Headley, IVUN, and Consultant to the Home-Based Mechanical Ventilation and Neuromuscular Disease NetWork
Networking
Resources for “Transitioning”
Since 2000, the HEATH Resource Center has served as a national clearinghouse on postsecondary education for individuals with disabilities, managed by The George Washington University Graduate School of Education and Human Development. Now, The HSC Foundation has partnered with The George Washington University to expand the content of this resource and to designate it as the official site of The HSC Foundation's National Youth Transitions Center.
HEATH participates in national conferences, training sessions, and workshops; develops training modules; publishes resource papers, fact sheets, directories, and website information; and fosters a network of professionals in the arena of disability issues.
Their latest publication, 2015-2016 Planning Ahead: Financial Aid for Students with Disabilities, addresses the fact that “while education beyond high school in the United States is optional, it has become a necessary investment in future employment and life satisfaction for many people. Most, however, cannot afford to make this investment without some outside monetary assistance. Over the years, public and private sources of money have been developed specifically to meet this need.”
HEATH responds annually to thousands of electronic mail. Interested in postsecondary education and training? Visit HEATH’s Frequently Asked Questions or send specific questions to askheath@gwu.edu.
Update on ABLE Act
The ABLE Act amends Section 529 of the Internal Revenue Service Code of 1986 to create tax-free savings accounts for individuals with disabilities. The bill aims to ease financial strains faced by individuals with disabilities by making tax-free savings accounts available to cover qualified expenses such as education, housing and transportation. The bill supplements, but does not supplant, benefits provided through private insurances, the Medicaid program, the supplemental security income program, the beneficiary’s employment and other sources.
Connect here to find the details of implementation of the ABLE ACT in your state.
New home-care worker pay rules cleared
Posted October 6th, 2015, on SCOTUS BLOG
Chief Justice John G. Roberts, Jr., on Tuesday afternoon cleared the way for home-care workers who are hired by businesses to be eligible for minimum wages and overtime pay, beginning next Tuesday. The Chief Justice signed a simple order, without explanation, denying a request by three home-care industry groups for a delay of new Labor Department rules. He acted alone and without seeking a reaction from the department.
Last month, the industry groups, arguing that the new rules would lead to the loss of home care for millions of elderly and disabled individuals, sought a delay until they could file a challenge to a decision by the U.S. Court of Appeals for the District of Columbia Circuit, upholding the rules.
For decades, the Labor Department had followed a policy that home-care workers were not eligible for minimum wage and overtime pay provisions of federal law. Two years ago, it changed its mind, concluding that the home-care industry had changed markedly, with fewer patients being treated in nursing homes and hospitals and more receiving care at home.
The new rules do not apply to home-care workers who are hired directly by patients or their families, but only to those who are employed through businesses. The rules will go into effect when the D.C. Circuit issues the formal order implementing its August 21 decision. The industry groups filed their postponement request with Roberts because he handles emergency filings from the D.C. Circuit.
The Chief Justice’s order simply turned down a request to postpone the implementation of the rules. The industry groups had said they would be filing a full appeal to challenge the changes. The Chief Justice’s order does not necessarily mean that such an appeal, if it is now filed, would be turned away, but one of the factors in deciding for or against a delay of a lower court order is whether the Supreme Court is likely to take on the issue.
Advocacy
NAMDRC tackles archaic home mechanical ventilation Medicare rule
Ever wonder why your "breathing machine” is called a ventilator by your physician and at other times it is called a respiratory assist device or RAD? The answer is about as confusing as the question. Medicare does not recognize the Food and Drug Administration classification of devices as ventilators. Therefore, while one agency within the Department of Health & Human Services is specifically charged with the responsibility for determining safety and efficacy of medical devices and providing strict rules for labeling (FDA), a sister agency (Medicare) in the same department is not bound to accept those determinations. This has the effect of Centers for Medicare and Medicaid Services stating that "just because FDA calls a device a ventilator does not make it a ventilator.”
NAMDRC (National Association for Medical Direction of Respiratory Care) is trying to clarify and correct this confusion and develop solutions that will stand the test of time by building in flexibility. As NAMDRC explains in CHEST Physician, September 2015, "We see little need to distinguish between invasive and noninvasive home mechanical ventilation for coverage purposes. The principle outlined in the 2001 Decision Memo is outdated and no one genuinely believes that, by definition, the most critically ill must have a trach in order to survive. Let the physician determine the best approach; and in the case of many patients, particularly in the neuromuscular arena, a patient might use invasive mechanical ventilation nocturnally and noninvasive ventilation at other times. Importantly, most devices today can accommodate either approach.”
Asked to sign petitions regarding CRT?
What is CRT? Complex Rehab Technology
What is the issue? Best described here by the Paralyzed Veterans Association, these items were exempted from inclusion of Medicare's new DME competitive acquisition program. However a separate CRT benefit structure was not established at that time. Advocacy groups are asking that Congress pass the "Ensuring Access to Quality Complex Rehabilitation Technology Act,” a bipartisan bill that will create a separate benefit category for complex rehab technology. For details and to "Take Action,” see The Advocacy Center of United Spinal Association.
Ventilator Users Speak
The Heartful Mom
The Heartful Mom is the blog of Lori, who with her husband Kevin, have four children, two of which have an extremely rare genetic disorder - Warburg Micro Syndrome.
MaryEllen is 28 years old. Kevin is 27. They are the oldest known individuals in the world with Warburg Micro syndrome.
Lori writes, “They both require a wheelchair, special bed, tube feedings, a ventilator, numerous medications and around the clock care.
“As they got older, their medical needs became more complex. Even though it may seem like they don’t understand what is going on around them, they most certainly do. They communicate by facial expressions and head nods. Their body language also conveys their moods and likes and dislikes.”
In a recent blog, “Three Cheers For Strong Moms Everywhere,” Lori comments, “Let’s stop comparing and judging and let’s just love our kids. We’re all in this together and the most precious commodity of our generation is our children.”
To receive notifications of new posts by email, sign up at the bottom of the page at The Heartful Mom.
Lauren Scrivo
Ventilator user Lauren Scrivo, MA, a Senior Communications Specialist at Kessler Foundation, visited Franklin D. Roosevelt’s childhood home and opines: “Eighty years later, how much has changed?
“I was born with my disability. Having a form of muscular dystrophy, I needed a ventilator to breathe since I was a year old and in a power wheelchair a year later. Fortunately, I’m part of the “ADA Generation.” I entered kindergarten the September following the signing of the Americans with Disabilities Act (ADA), which mandated public schools to be made accessible. Curbs and steps turned to ramps.”
Her thoughts are found at the Real Economic Impact Blog of the National Disability Institute.
Recent Relevant Publications
Enrollment in Diaphragm Pacing Systems for People with ALS Halted
The ALS Association
“…Data Safety and Monitoring Board (DSMB), constituted to oversee the Diaphragm Pacing System in Participants with Amyotrophic Lateral Sclerosis (DPS in ALS) study, being conducted in the United States, issued a recommendation that new enrollment be halted. At the same time, the DSMB recommended that patients already randomized to the diaphragm pacing arm continue to be actively stimulated and followed according to the protocol.” Read more.
Severe respiratory illness associated with a nationwide outbreak of enterovirus D68 in the USA (2014): a descriptive epidemiological investigation
Claire M Midgley, John T Watson, W Allan Nix, Aaron T Curns, Shannon L Rogers, Betty A Brown, and others in The Lancet Respiratory Medicine, published online: October 5, 2015.
“…145 (28%) of 511 received ventilator support.”
“In 2014, EV-D68 caused widespread severe respiratory illness across the USA, disproportionately affecting those with asthma. This unexpected event underscores the need for robust surveillance of enterovirus types, enabling improved understanding of virus circulation and disease burden.” Read more.
Respiratory Health and Spinal Cord Injury
Eric Garshick, MD, MOH, Phil Klebine, MA, Daniel J. Gottlieb, MD, MPH, and Anthony Chiodo, MD in collaboration with MSKTC (Model Systems Translation Center).
“Signals sent from your brain can no longer pass beyond the damage to the spinal cord, so your brain can no longer control the muscles that you would normally use for inhaling and exhaling. The extent of your muscle control loss depends on your level of injury and if there is complete or incomplete spinal cord damage. If you have a complete high cervical injury that involves the spinal cord at or above the cervical 3rd, 4th, and 5th spinal nerves, you may have a loss of or weakness in diaphragm function depending on the extent of damage.” Read more.
A comparison of high vs standard tidal volumes in ventilator weaning for individuals with sub-acute spinal cord injuries: a site-specific randomized clinical trial
M L Warner, D Lammertse, S Charlifue, L Martinez, A Dannels-McClure, S Kreider and C Pretz in Spinal Cord, September 15, 2015.
“…we report the safety outcomes of 33 study participants. The 16 patients in Group 1 and 17 patients in Group 2 were demographically similar at baseline, except for age. Conclusion: Higher tidal volumes can be safely utilized during weaning of patients with tetraplegia from mechanical ventilation using a 14-day weaning protocol.” Read more.
Family Caregiving: 20 Years of Federal Policy
From In Focus by Mathematica Policy Research
“Family caregivers are a hidden workforce that is essential to meet the growing demand for long-term services and supports by older adults and people with disabilities. Yet the policies and programs available in the United States are much less supportive than those in most other developed countries….” Read more.
Why dozens of "vent kids" stuck in Washington hospitals can’t go home
Levi Pulkkinen, seattlepi.com Staff on seattlepi.com, Thursday, October 15, 2015
“A federal lawsuit has been filed on behalf of five Washington children who need ventilators to live. Here are the key claims: 1) These children and dozens of others could be living at home if the state, through Medicaid, would provide nursing care; 2) Low Medicaid reimbursement rates have made it nearly impossible for nursing agencies to hire and retain skilled home care nurses; 3) Federal disability law requires that Washington come through with nurses for Medicaid-insured children.” Read more.
Educational Opportunities
AARC Congress 2015 in Tampa
November 7 - 10, 2015, American Association for Respiratory Care (AARC) Congress 2015, The 61st International Respiratory Convention & Exhibition, Tampa, Florida.
Swiss Paraplegic Centre
November 26 - 27, 2015
8th Scientific Symposium ‘Life and Care’ Weaning/Breathing,
Swiss Paraplegic Center, Nottwil, Switzerland.
Canadian Respiratory Conference (CRC) 2016
April 14-16, 2016, World Trade and Convention Centre, Halifax, Nova Scotia, Canada. More.
CHEST World Congress 2016
April 15-17, 2016, Shanghai, China, English | 中文,
Download the Preliminary Program.

Parent Project Muscular Dystrophy
June 26-30, 2016, 2016 Annual Connect Conference - Orlando, Florida. PPMD is offering a scholarship program to waive registration fees for families who have been diagnosed after January 2015.
European Respiratory Society (ERS) International Congress 2016
September 3-7, 2016, London, United Kingdom. More.
Industry
New app for iPhone and iPad
The Passy Muir® TRACHTOOLS™ Speech & Resources App features pre-recorded responses and phrases to enable communcation at a touch of a button. The user can choose a male or female voice and it also has a child voice option. The app is easy to use and provides links to useful resources and patient videos.
New from Philips Respironics
DreamWear is a new under the nose nasal mask marketed for CPAP (vented). The tubing attachment is located at top of head. The soft, flexible silicone frame and fabric wrap is soft on the cheeks. The air is delivered to the nose through the silicone frame. It is available in small, medium, large, medium-wide. Check out the DreamWear Brochure.





